Content table
Can vulvodynia cause infertility? It’s a question that affects more women than you might think.
Research estimates show that 10-28% of women experience vulvodynia, and in the U.S., that’s around 13 million people (16%). It most commonly affects women between the ages of 18 and 25.
The good news: vulvodynia does not directly cause infertility. But its effects on sexual function can indirectly reduce a couple’s chances of conceiving. And that’s worth understanding.
If you’re living with persistent vulvar pain and wondering what it means for getting pregnant, this article is for you.
Key Takeaways
- Vulvodynia is a chronic pain condition — persistent pain in the vulvar region lasting at least 3 months with no clear cause.
- Vulvodynia does not directly cause infertility. But it can make conception harder by affecting how often and how comfortably you have sexual intercourse.
- Painful intercourse is one of the most significant challenges women with vulvodynia face when trying to conceive. Studies show 58% of affected women stopped having sex because of vulvodynia symptoms.
- Anxiety, stress, and relationship strain also reduce sexual frequency — and can affect ovulation.
- Vulvodynia diagnosis is a process of ruling out other causes first, including infections, skin conditions, and sexually transmitted diseases.
- A full infertility evaluation should be done to rule out other medical reasons before linking conception difficulties to vulvodynia.
- With the right treatment plan — including pelvic floor therapy, pain management, and smart fertility tracking — most women with vulvodynia can still conceive.
What Is Vulvodynia?
Vulvodynia is a chronic vulvar pain condition. It is defined as “vulvar pain of at least 3 months’ duration, without a clear identifiable cause, which may have potential associated factors” by The International Society for the Study of Vulvovaginal Disease (ISSVD). This terminology is now widely used by doctors around the world.
In simple terms, it’s ongoing pain in the vulvar area (the external female genitals) that has no obvious explanation. No infection. No skin condition. No sexually transmitted disease. Just pain that won’t go away, often for long periods of time.
The pain can be localized vulvodynia — focused in one area, like the vaginal opening or clitoris. Or it can be generalized — spread across the whole vulvar region. Women with localized vulvodynia often experience pain only in response to touch or pressure, while those with generalized vulvodynia may feel it constantly.
Vulvodynia is also categorized as:
- Primary: Present from the very start, with no pain-free period before
- Secondary: Pain that develops later, such as after a procedure, or hormonal changes
What Are the Most Common Symptoms of Vulvodynia?
The most common symptoms of vulvodynia include:
- A burning sensation in the vaginal area
- Rawness, stinging, or aching in the vulvar region
- Increased sensitivity or soreness in the female genitals
- Pain during or after sexual intercourse
- Pain triggered by touch, pressure, or sitting for long periods
In some women, these symptoms may overlap with those of other conditions, such as yeast infections or contact dermatitis. That’s part of why vulvodynia so often goes undiagnosed.
What is clitorodynia?
Clitorodynia is a specific subtype of vulvodynia. It causes intense pain localized to the clitoris that’s often described as:
- A burning sensation
- Rawness
- Feeling of pressure
The pain can happen on its own. Or it can be triggered by touch, pressure, or sexual activity. The clitoris plays a key role in sexual arousal and has a high concentration of nerve endings. This means that clitorodynia can make sexual intercourse extremely difficult, which compounds its impact on reproductive health and fertility.
What causes vulvodynia?
Researchers don’t have one clear answer yet. The exact risk factors are still being studied. But most evidence points to a multiple causes, including:
- Nerve irritation or increased sensitivity
- Hormonal imbalances
- Inflammation
- Genetic factors
- Pelvic floor muscle dysfunction
- Abnormal responses to certain triggers
One thing is clear: vulvodynia is not caused by infection or anything you did wrong. It’s a recognized chronic pain condition, and one that’s been widely underdiagnosed in the general population.
How common is vulvodynia?
Research shows that 10-28% of women will experience vulvodynia at some point. It’s most common in women aged 18-25, though women of all ages can be diagnosed with this condition.
Despite how common vulvodynia is, many women go years without a proper diagnosis. Research shows that 60% of affected women consult at least three doctors before getting answers. And 40% remain undiagnosed even after three visits!
That’s a long time to live with pain and no answers, especially if you’re trying to start a family.
How Does Vulvodynia Affect Fertility?
Vulvodynia doesn’t damage the reproductive system. But it creates significant challenges for women trying to conceive naturally. Here’s how.
1. Painful intercourse (dyspareunia)
This is the most direct connection between vulvodynia and fertility.
When sexual intercourse is painful, couples have it less often. Some stop altogether. That means fewer opportunities to conceive, especially if intercourse is avoided during the fertile window.
The associated sexual pain may lead to avoidance or interruption of intercourse, and this directly affects the timing needed for natural conception. Studies confirm that women with vulvodynia say persistent vulvar pain significantly disrupts sexual activity.
The ongoing stress and worry that come with this pain syndrome also affect sexual relationships and pregnancy planning. This adds more pressure on couples who are already working hard to conceive.
2. Reduced sexual activity
One study found that chronic vulvar pain had a moderate to severe impact on sex life in 45% of cases. Vulvodynia pain caused 58% of women to stop having sexual intercourse altogether. And almost half of all cases avoided sexual relations because of their vulvodynia symptoms.
Regular intercourse is essential for natural conception, and your fertile window is only about 6 days per cycle. So even a moderate reduction in frequency can meaningfully lower your chances of getting pregnant.
Know more: Getting Pregnant: When Are You Most Fertile?
3. Psychological factors
The impact of vulvodynia goes far beyond the physical vulvar pain.
Research shows that women with vulvodynia experience higher levels of:
- Anxiety
- Psychological distress
- Reduced relationship satisfaction
When compared to women without the condition. Fertility-related stress was also notably higher in women diagnosed with vulvodynia.
These factors matter for conception too. Chronic stress raises cortisol (your stress hormone), which can interfere with the hormonal signals that trigger ovulation.
Sexual dysfunction linked to vulvodynia pain isn’t just a physical problem. It’s an emotional and relational one too.
How Is Vulvodynia Diagnosed?
Vulvodynia diagnosis is made through a process of exclusion. This means other identifiable causes of vulvar pain must be ruled out before a doctor can confirm vulvodynia.
Conditions that doctors typically check for first include:
- Yeast infections and other vaginal infections
- Sexually transmitted diseases
- Skin conditions in the vulvar area
- Lesions or growth
Doctors use both clinical assessment and targeted tests as exclusion criteria to rule out underlying conditions before arriving at vulvodynia diagnosis.
How Do Doctors Rule Out Other Causes of Infertility?
Before linking difficulty conceiving to vulvodynia, doctors first look for common biological causes of infertility. This is an important step, and one that many women skip.
According to WHO-supported guidelines, a standard infertility evaluation includes:
- Ovulation check: Are you ovulating regularly?
- Hormone testing: FSH, LH, estrogen, progesterone, and AMH levels
- Uterine and fallopian tube assessment: Are there structural issues?
- Semen analysis: Checking for signs of male infertility
A comprehensive review of medical history, along with a careful physical assessment are also part of this process. They help doctors identify any underlying conditions and decide which tests are most relevant.
Only when all investigations come back normal — and no clear biological cause is found — is infertility labeled as “unexplained.” At that point, functional factors like vulvodynia become more clinically relevant. This is especially true when painful sex has been reducing or stopping sexual intercourse during the fertile window.
Know more: Fertility Tests for Women
How Do You Manage Vulvodynia When Trying To Conceive?
Managing vulvodynia takes a comprehensive, multidisciplinary approach that combines medical treatment, physical therapy, and mental health support.
Here’s what that looks like in practice.
Avoid triggers
Many women with vulvodynia find relief by identifying and removing things that make their symptoms worse:
- Harsh soaps, scented products, or chemicals near the vaginal area and vaginal opening
- Tight clothing or synthetic fibers
- Sitting for long periods without a break
Switching to loose, breathable cotton underwear can make a meaningful day-to-day difference.
Pain relief treatments
The right treatment for vulvodynia depends on the type and the severity of pain. Most women with vulvodynia will need a combination of approaches to get real relief. Common options include:
- Topical numbing cream or gels (like lidocaine): Applied before sex to reduce pain
- Hormone-based creams: Helpful when hormonal imbalances are part of the cause
- Oral medications: Nerve pain drugs, antidepressants, or anticonvulsants can reduce vulvodynia pain in many women
- Nerve blocks or minor procedures: Considered for specific, consistent cases
The National Vulvodynia Association is one of the best resources for women diagnosed with vulvodynia who are looking for treatment, guidance, provider recommendations, and community support.
Always work with a doctor who has experience with vulvodynia to find the right treatment for your situation.
Physical therapy
Pelvic floor therapy is one of the most evidence-backed treatments for vulvodynia.
Many women with this condition have tight or overactive pelvic muscles and vaginal muscles. This muscle tension makes sexual intercourse more painful. A trained pelvic floor therapist uses targeted exercises, biofeedback, and hands-on techniques to relax these muscles over time.
For most women with vulvodynia, consistent physical therapy leads to improvement in vulvodynia symptoms, and a gradual return to comfortable sexual intercourse. It’s often one of the most important parts of managing vulvodynia long-term.
Mental health and counseling support
The mental health toll of living with chronic pain is real and it deserves attention.
Women suffering from vulvodynia often deal with anxiety, depression, and relationship strain on top of physical pain. Techniques like mindfulness, relaxation exercises, and cognitive behavioral therapy (CBT) all help with managing vulvodynia’s emotional side.
Couples counseling is also worth considering. Open, honest conversations about pain, intimacy, and fertility goals help partners feel like a team rather than isolated in the struggle.
What Fertility-Focused Tips Can Help Women With Vulvodynia?
Managing vulvodynia while trying to conceive takes patience and a thoughtful approach. Here’s what can help.
Maintain intimacy
Sexual pain can make penetrative sex feel out of reach. But intimacy doesn’t have to stop.
Non-penetrative options like mutual touch, sensual massage, or other forms of physical closeness that feel comfortable help you and your partner stay connected.
Focus on comfort first. A slow, gradual return to intercourse is always better than pushing through pain.
Time intercourse
You don’t need to have sex every day to get pregnant. But you do need to know when your fertile window is open and make those days count.
Your fertile window includes the 4 days before ovulation, the day of ovulation, and the day after ovulation. Sexual intercourse during that window, even if less frequent than usual, gives you a real shot at conception.
The key is knowing exactly when those days fall. That’s where hormone tracking makes a difference.
Rather than guessing based on calendar dates, tracking your actual hormones tells you what’s really happening in your body.
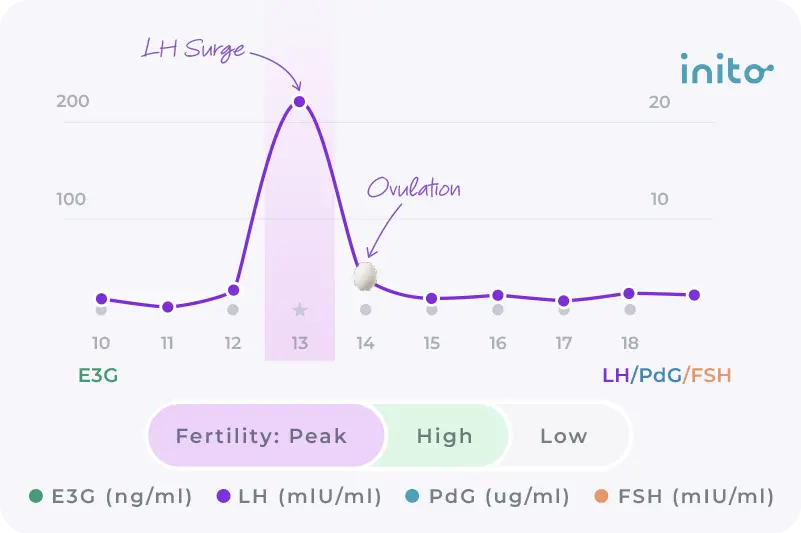
The Inito Fertility Monitor tracks all four fertility hormones — estrogen, LH, PdG, and FSH — on a single test strip in just 10 minutes. With Inito, you can:
- Identify your fertile days
- Know when ovulation is coming
- Confirm that ovulation actually happened through a sustained PdG rise
For women with vulvodynia who need to make every opportunity count, that kind of clarity matters more than almost anything else.
Know more: When to Have Sex to Conceive
Make intercourse more comfortable
When sexual intercourse is possible, these steps can help reduce pain:
- Try when vulvodynia pain is at its lowest. For some women, this may be in the morning. But the best time differs from woman to woman.
- Use plenty of lubrication.
- Ensure full arousal before penetration.
- Choose positions that reduce pressure on the vaginal opening.
- Use supportive pillows to reduce strain on the pelvic muscles.
- Limit thrusting and move slowly.
- Apply a topical anesthetic 20-30 minutes before intercourse if your doctor recommends it.
Consider infertility treatment options
For women who find penetrative sex too painful even with treatment, infertility treatment options are available that don’t require intercourse at all.
Timed intrauterine insemination (IUI) is one fertility treatment that bypasses the need for sexual intercourse entirely. If other fertility factors are also present, or if IUI hasn’t been successful, in vitro fertilization (IVF) may be the next step.
Fertility treatments like these have helped many women with vulvodynia build the families they want. Talk to a reproductive specialist about which infertility treatment makes the most sense for your situation.
The Bottom Line: Can Vulvodynia Cause Infertility?
Not directly. But vulvodynia can get in the way of getting pregnant, cycle after cycle via:
- Painful sex
- Missed fertile windows
- Emotional weight of chronic pain
The good news? It’s manageable. WIth the right treatment, pelvic floor therapy, and smart fertility tracking, most women with vulvodynia can still get pregnant.
You are not broken. You are not alone. And you don’t have to do this without support.

FAQs
Yes! Vulvodynia does not damage your reproductive organs. Your ovaries, uterus, and fallopian tubes are not affected by this condition.
In fact, many women with vulvodynia go on to have children. The goal is to manage the pain well enough to have sexual intercourse during the fertile window, or exploring fertility treatments like IUI if intercourse is too painful.
The three most common causes of female infertility are:
- Ovulation problems (like those caused by PCOS or hormonal imbalances)
- Blocked or damaged fallopian tubes
- Uterine or cervical issues
Vulvodynia is not one of the top direct causes. But it can contribute to “unexplained infertility” when painful intercourse significantly reduces the frequency of sex during the fertile window.
Yes. Hormones may play a role.
Some women develop vulvodynia symptoms after hormonal changes, such as:
- Starting or stopping birth control
- Going through menopause
- Experiencing shifts in estrogen levels
Low estrogen in particular can cause thinning and dryness in the vaginal area, which may worsen vulvar pain. If you suspect a hormonal link, talk to your doctor about testing your hormone levels.
Yes! Vulvodynia does not directly prevent pregnancy. But it can make conception harder when pain leads to less frequent sexual intercourse, especially during the fertile window.
With the right vulvodynia treatment and hormone tracking, most women with vulvodynia can still conceive naturally.
For those who can’t tolerate penetrative sex, fertility treatments like IUI or IVF are also effective options.
Research is still looking into whether PCOS and vulvodynia are linked. But no direct connection has been found yet.
What we do know is that some women with either condition experience hormonal imbalances. These can affect genital tissue sensitivity and sexual function.
If you have PCOS and vulvar pain, it’s worth talking to a gynecologist who knows both conditions well.
Know more: Common PCOS Treatment Options for Better Fertility
Yes. A gynecologist is usually the first doctor women with vulvodynia see. They can diagnose the condition by ruling out other causes of vulvar pain and recommending a treatment plan.
For the best results, look for a gynecologist who has specific experience with vulvodynia.
Was this article helpful?
Vulvodynia (chronic vulval pain) | PMC
Understanding Vulvodynia | National Vulvodynia Association
Approach to Evaluation and Management of Infertility | NCBI Bookshelf
Vulvodynia Treatments | National Vulvodynia Association
Overcoming Challenges in Your Intimate Relationship | National Vulvodynia Association