Content table
Hoping to get a better understanding of your PCOS hormone levels and fertility? With PCOS impacting up to 13% of women globally, you’re not alone.
Polycystic ovary syndrome (PCOS) is also the number one cause of anovulation. So it’s no wonder that 90–95% of women seeking fertility treatment for anovulation have PCOS.
You’re in the right place for all these concerns, though. In this article, you’ll get a close-up of how PCOS affects your levels of androgens, insulin, LH, and more.
So keep reading for helpful PCOS hormone levels charts as well as what it all means for your fertility.
Key Takeaways
- Polycystic ovary syndrome (PCOS) is a condition that causes hormonal imbalances that affect a woman’s ovarian function.
- Women with PCOS have higher amounts of androgens (male sex hormones) like testosterone.
- PCOS also causes an increase in insulin levels and luteinizing hormone levels which can lead to disruptions with ovulation.
- The LH to FSH ratio can also be slightly increased if you have PCOS.
- Women with PCOS usually have higher levels of Anti-Müllerian Hormone (AMH).
- PCOS can lead to estrogen dominance (when there’s a higher amount of estrogen to progesterone).
- Some women with polycystic ovarian syndrome (PCOS) may have elevated prolactin levels.
- Even though PCOS throws many of these hormones out of whack, it’s still possible to get pregnant.
- If you have PCOS and you’re trying to conceive, track your cycle to see if you are ovulating or not. You can also consult with your doctor about a gameplan for your diet and exercise.
What is PCOS?
Polycystic ovary syndrome (PCOS) is a condition that causes hormonal imbalances that affect ovarian function.
The three major marks of a PCOS diagnosis include having:
- Multiple cysts on the ovaries
- Irregular ovulation or anovulation (no ovulation)
- Elevated levels of androgens (male sex hormones)
Lots of research has been done to further explore PCOS, but the root cause of the condition is still unknown. Researchers believe it’s a result of both genetic and environmental factors. They also believe a family history of the condition plays a part as well.
No matter the cause, though, we do know that PCOS causes abnormal levels of certain hormones. Learn more about how this happens next.
How Does PCOS Affect Hormones?
PCOS disrupts the typical production of multiple hormones. For starters, the majority of those with PCOS have increased amounts of androgens, insulin, and luteinizing hormone (LH).
But other hormones like FSH, AMH, progesterone, estrogen, and prolactin can be affected as well.
To get a better sense of how each hormone is uniquely affected by PCOS, take a look at the charts that follow.
PCOS and androgen levels
Roughly 60% of women with PCOS have hyperandrogenism, aka an excess of androgens. Androgens is an umbrella term that refers to a number of male sex hormones like testosterone and androstenedione.
Why does this imbalance happen?
In PCOS patients, the ovaries (and sometimes the adrenal glands) produce extra androgens. These excess androgens go unregulated by other hormones.
Unchecked androgen levels are further encouraged to keep climbing when insulin resistance and hyperinsulinemia exist. This is because elevated androgens lead to lower amounts of sex hormone-binding globulin (SHBG) levels. (SHBG typically helps stabilize androgen levels by binding to them and keeping them from roaming freely.)
See the image below for a visual of how PCOS androgen levels compare to non-PCOS levels.
PCOS insulin levels and insulin resistance
Studies have observed a clear correlation between insulin levels and PCOS testosterone levels.
Between 50% and 70% of PCOS patients have insulin resistance. (This is why researchers believe high insulin levels to be one of the culprits for the initial development of the disease).
Why causes these higher-than-normal insulin levels?
Women who have insulin resistance are likely to experience disrupted production of sex hormone-binding globulin (SHBG). This interference then causes a spike in testosterone levels which can mess with ovulation and cause irregular menstrual cycles.
When ovulation is disrupted, other hormones get thrown out of whack. And then the cycle of high androgens continues.
Look at the chart below to see how PCOS insulin levels compare to non-PCOS levels.
PCOS and luteinizing hormone (LH)
Another typical hormonal imbalance common in polycystic ovary syndrome is high luteinizing hormone (LH) levels. Close to 3 in 4 PCOS patients have LH levels above the 95th percentile.
When you have too much LH, it can keep your ovarian follicles from developing properly. This can then cause problems with ovulation and fertilization.
Why does this imbalance happen?
PCOS speeds up the pulsating production of gonodatropin-releasing hormones (GnRH). Since GnRH is what triggers LH secretion, LH levels increase beyond what they’re supposed to.
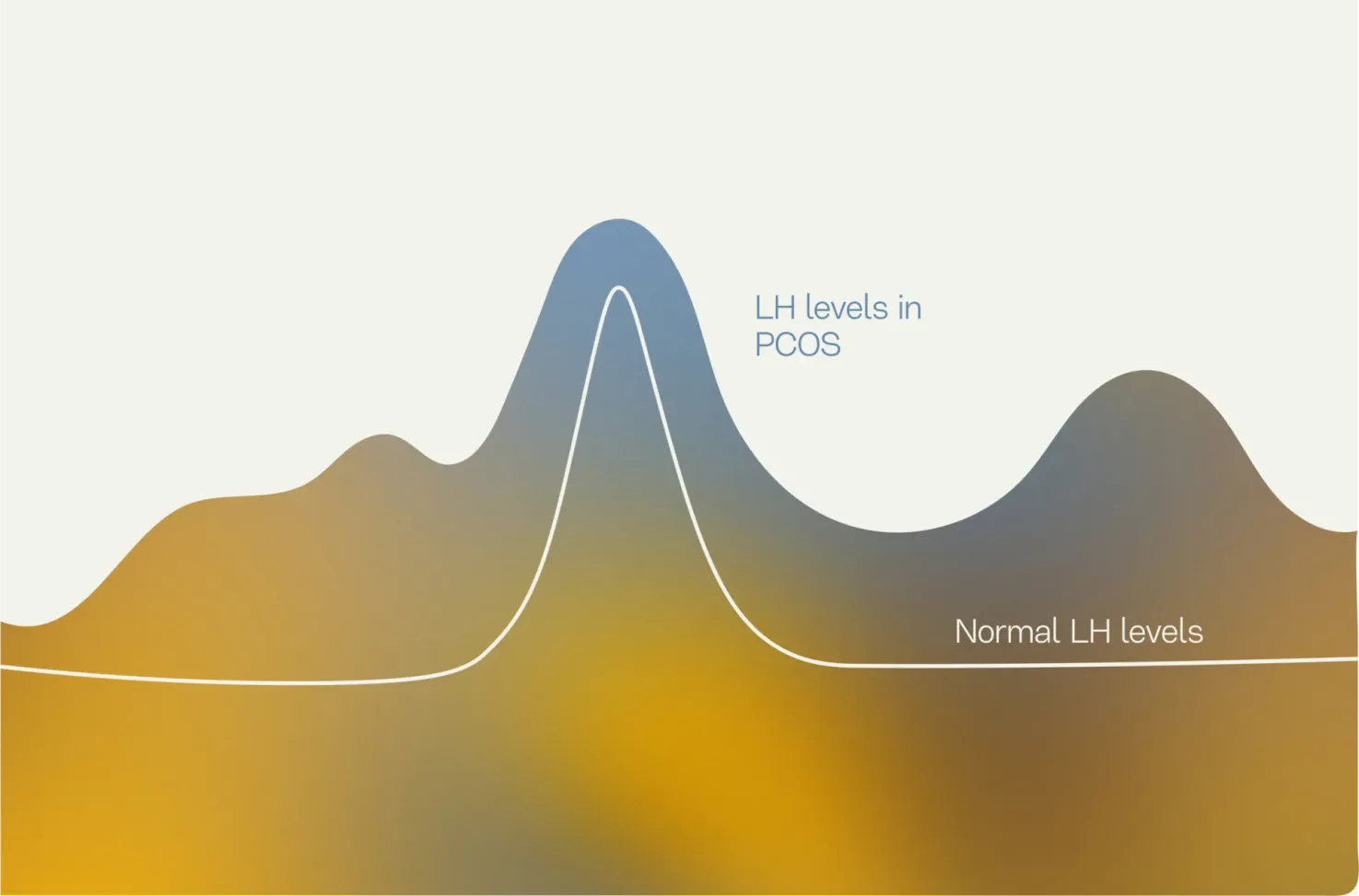
In a healthy menstrual cycle, your LH levels should spike right before you ovulate. But for many women with PCOS, LH levels tend to creep up at random times throughout their menstrual cycle.
Know more: High LH Levels: Common Causes and Next Steps
Look at the LH levels chart below to compare PCOS LH levels versus normal LH levels in females.
PCOS and follicle-stimulating hormone (FSH) & the LH/FSH ratio
There are conflicting findings when it comes to follicle-stimulating hormone levels and PCOS. Some reports indicate that FSH levels are normal or slightly lower because of how GnRH is disrupted. But other studies observe elevated levels of FSH in those with PCOS.
That said, nearly 60% of PCOS experience an increased LH to FSH ratio of 2:1 or 3:1. In a normal menstrual cycle, the LH: FSH ratio is 1:1 or 2:1 around the time of ovulation.
Why does this imbalance exist?
As of now, there’s no fully proven reason for how PCOS impacts follicle-stimulating hormone levels. But researchers believe it could be a result of how the pulsating pattern of GnRH production is disrupted.
Know more: What Your FSH & LH Ratio Says About Your Fertility
Look at the chart below for a visual of how the PCOS LH FSH ratio is impacted.
PCOS and Anti-Müllerian Hormone (AMH)
One study looked at AMH levels in over 600 PCOS patients. It revealed a tight connection between AMH levels and conventional criteria for diagnosing PCOS.
Another study found that more than 97% of women with ultrahigh AMH (levels greater than 10 ng/mL) had PCOS.
Why does this AMH imbalance exist?
As mentioned, the high LH levels that come with PCOS can keep ovarian follicles from maturing properly. This leads to PCOS patients also having a higher amount of antral follicles (small sacs that contain immature eggs).
Antral follicles are responsible for producing AMH. So because there are more of them than there should be, women with PCOS are likely to have elevated AMH levels.
Look at the chart below to see how AMH levels look for PCOS patients.
PCOS and progesterone
Since PCOS can cause less frequent or absent ovulation, women with PCOS may have unusually low progesterone levels.
Why does this happen?
When you ovulate, the follicle that released the egg forms the corpus luteum. Its main job? Produce progesterone to support a potential pregnancy.
If you don’t ovulate, then the corpus luteum never forms, which means your body won’t produce progesterone.
Know more: Daily Progesterone Levels After Ovulation: What to Expect
PCOS and estrogen
There’s a bit of variance in estrogen levels for women with PCOS. For some, estrogen levels may be normal. But for others, they may be lower or higher than normal.
There is one thing that seems to be true across the board for PCOS women though. It’s that there’s some degree of estrogen dominance due to having a higher estrogen to progesterone ratio.
Know more: Estrogen Dominance and How Does It Affect the Body?
PCOS and prolactin
A final hormone that is sometimes impacted in women with PCOS is prolactin. Studies show that for up to 30% of those with PCOS, there’s a slight rise in prolactin levels during the follicular phase and luteal phase.
Why does this imbalance happen?
The exact relationship between PCOS and prolactin is still being explored. But it’s possible that it’s tied to insulin resistance and a sped up GnRH release pattern.
Know more: Prolactin and Fertility: Causes of High Levels and Solutions
With all of these hormones operating differently, you may be concerned about what this means for your fertility as a PCOS patient. So keep reading to get some of your most pressing questions answered!
Can You Still Get Pregnant With PCOS?
Yes!
While the condition can make it more challenging to conceive, you can still get pregnant with PCOS.
PCOS plays an integral role in your hormone levels and metabolic system. So there are actually quite a few ways you can manage symptoms that would impact your fertility.
If you have PCOS and you’re trying to conceive, your major priorities should be to:
1) Restore ovulation
2) Regulate your periods
3) Manage insulin resistance
If that sounds a bit abstract still, not to worry! Here are some concrete ways you can work towards those three goals:
- Adopt a nutritious, hormone-balancing diet
- Talk to your doctor about healthy and sustainable ways for losing weight (if your BMI is too high)
- Get regular moderate exercise
- Keep your levels of stress in check (high stress can interrupt hormonal function)
- Track your menstrual cycles so you know if you’re ovulating or not
Download our PCOS Handbook Now
How can you tell if you’re actually ovulating?
There are several ways women check for ovulation. Some include tracking your basal body temperature or using ovulation predictor kits (OPKs). But for women with PCOS, these methods tend to be less reliable since hormone levels don’t function quite the same.
So if you have PCOS, using a more advanced ovulation tracking method like the Inito Fertility Tracker can be really helpful. With Inito, you get exact numeric values for your four key fertility hormones: estrogen, LH, PdG, and FSH.
By focusing on patterns over time rather than single spikes, Inito helps women with PCOS better understand when their fertile window truly begins, identify their true LH surge, and determine whether ovulation actually happened.
Know more: Real Stories of PCOS Insights From 250+ Inito Users
FAQs
A variety of factors lead to a woman having higher levels of testosterone. One of the most common reasons is polycystic ovary syndrome (PCOS). One of the hallmark signs of PCOS is having an excess of male sex hormones called androgens. And testosterone is an androgen.
Another potential factor could be congenital adrenal hyperplasia. If you’re concerned about your testosterone levels though, consult your doctor. They can help run some diagnostic testing and look at your medical history to pinpoint the root cause.
For some PCOS patients, yes it does. About 60% of women with PCOS experience hyperandrogenism (high levels of androgens), and testosterone is an androgen.
You’ll want to consult a healthcare professional about this. They will help you determine the root cause of not having sufficient LH levels around the time of ovulation. This can then inform your treatment plan.
No, female masturbation does not cause PCOS. Researchers are still at work trying to uncover the underlying root cause of PCOS. But it’s likely due to genetic and environmental factors.
There’s no singular blood test you would take to be diagnosed with PCOS. But getting bloodwork can help your doctor see your levels of certain hormones like LH and FSH as well as insulin. A blood test could also help rule out other potential conditions. So if you think you have PCOS, be sure to consult with your doctor.
Studies have reported that some women with PCOS have higher levels of DHEA (dehydroepiandrosterone sulfate). But this isn’t the case for most PCOS patients, so DHEAS levels aren’t considered a main factor in diagnosing PCOS.
Was this article helpful?
Elevated and diagnostic androgens of polycystic ovary syndrome – PMC
Role of Metformin in Polycystic Ovary Syndrome (PCOS)-Related Infertility – PMC
Diagnosis of Polycystic Ovary Syndrome: AMH in combination with clinical symptoms – PMC
Prolactin in Polycystic Ovary Syndrome: Metabolic Effects and Therapeutic Prospects
Is it Useful to Measure DHEAS levels in PCOS? – Science Direct