Content table
If you’re struggling to conceive, ovulation induction could be the answer you’ve been looking for.
Ovulation induction is a medical method that helps the ovaries release eggs. It works by fixing the hormonal signals between the brain and the ovaries. It does this via a system called the hypothalamic-pituitary-ovarian (HPO) axis so that ovulation can happen.
Ovulatory disorders cause about 25% of all infertility cases. Most of these are linked to PCOS. Another 15% of couples are told they have unexplained infertility, meaning no clear cause is found. Add those together, and nearly 40% of infertility cases could benefit from fertility treatments like ovulation induction.
That’s an estimated 19 million couples worldwide! Fortunately, there are effective treatments available.
Key Takeaways
- Ovulation induction is a treatment that helps the ovaries release eggs in women who don’t ovulate regularly or at all.
- The most common medications used are clomiphene citrate (Clomid®) and letrozole. Both are taken as oral medications early in the menstrual cycle.
- Letrozole tends to have higher ovulation and live birth rates than clomiphene, especially in women with PCOS.
- Injectable medications called gonadotropins are used when oral medications don’t work. They have the highest ovulation rates of all.
- Ovulation induction is often combined with timed intercourse or intrauterine insemination (IUI) to boost the chances of conception.
- Potential risks involve ovarian hyperstimulation syndrome (OHSS) and the possibility of multiple pregnancies. Both of these are reduced with careful monitoring.
What Is Induction of Ovulation?
Key Point: Ovulation induction uses medications to help the ovaries produce and release a mature egg.
Ovulation induction is a treatment used to stimulate the ovaries to develop and release eggs. It’s used for women who don’t ovulate regularly, or at all.
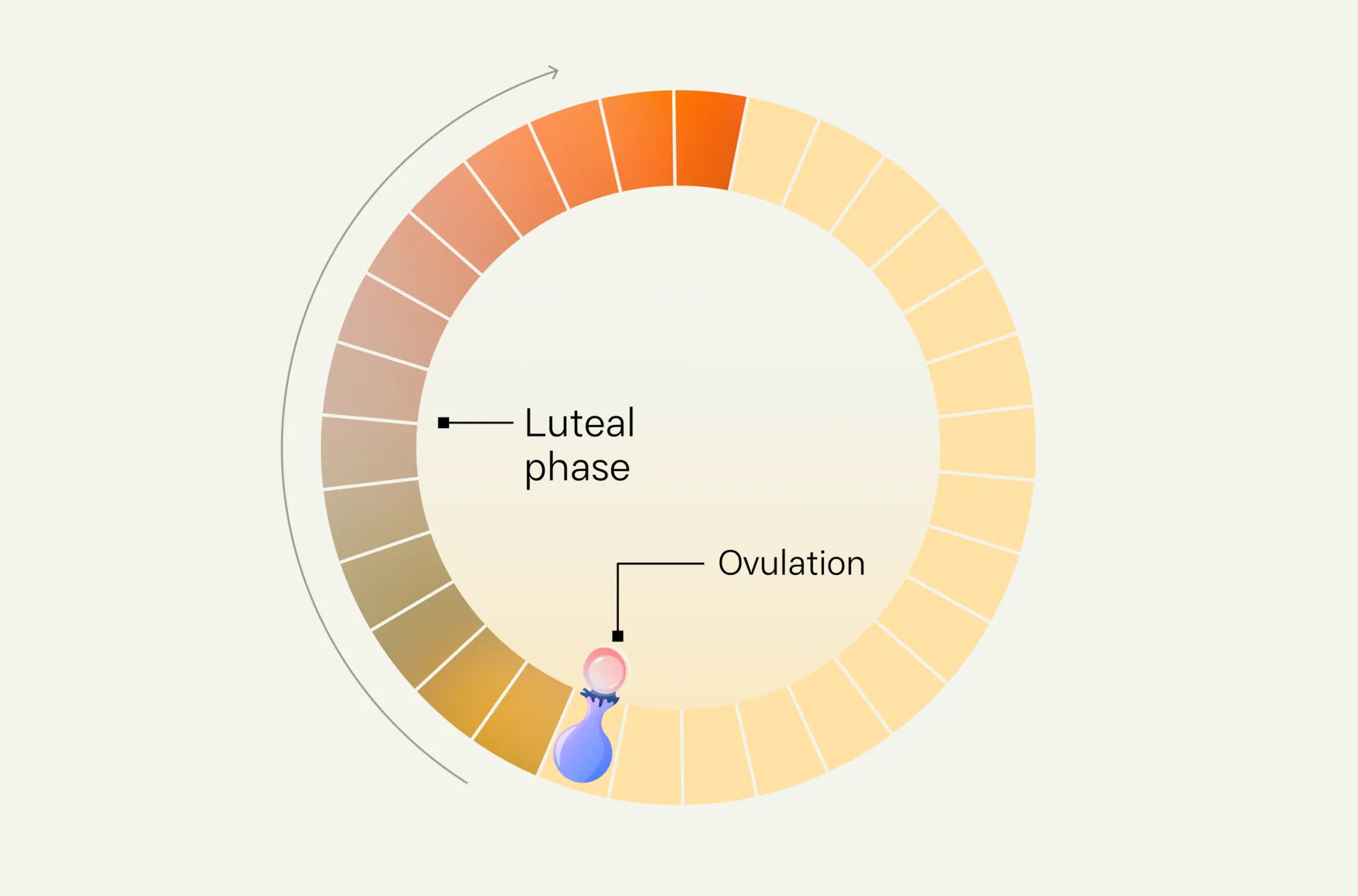
When a woman ovulates, her brain sends signals in the form of hormones to her ovaries. The ovaries respond by growing follicles (small fluid-filled sacs) and releasing an egg. That’s normal ovulation.
But when that signaling system breaks down, a woman ovulates irregularly or not at all. This is called anovulation, and it’s one of the most common causes of infertility.
Ovulation induction works by regulating those signals. Medications help stimulate follicle development and balance hormones.
They do this by:
- Modulating estrogen receptors
- Reducing androgen effects
- Improving insulin activity, or
- Directly stimulating the ovaries through gonadotropins
Know more: A Guide to Naturally Increasing Ovulation
Who Can Benefit From Ovulation Induction?
Key Point: Ovulation induction is most helpful for women who don’t ovulate regularly or at all.
Ovulation induction is recommended for women with:
- Anovulation or irregular ovulation
- Polycystic ovarian syndrome (PCOS)
- Unexplained infertility
- Luteal phase defects
- High prolactin levels (hyperprolactinemia)
- Poor response to fertility medicines for egg growth stimulation
- Prepping for IUI or assisted reproductive technology (ART)
It is not recommended when other major cases of infertility are present — things like blocked fallopian tubes or severe male factor infertility. In those cases, other treatments are needed first.
Know more: Identifying Infertility: Common Signs, Symptoms, and Causes in Men and Women
How Does Ovulation Induction Work?
Key Point: Ovulation induction uses a combination of lifestyle changes, fertility medications, and close monitoring.
Can lifestyle changes help you ovulate?
Yes! And they’re often the first step.
Research indicates that as little as 5-10% of body weight loss can help restore ovulation in some women with anovulatory PCOS.
- Improve hormonal balance
- Reduce androgen levels
- Make fertility medications more effective
Lifestyle changes alone won’t work for everyone. But they’re a low-risk starting point and they support any medical treatment you take.
Know more: A Guide to Naturally Increasing Ovulation
What Medications Are Used for Ovulation Induction?
Key Point: The medication options for ovulation induction are oral, injectable, and surgical. Each has different uses, success rates, and risks.
There are three main categories:
- Oral medications
- Injectable medications
- Surgical options
Let’s look at each one.
Oral medications
Clomiphene Citrate (Clomid®)
Clomiphene citrate is the most widely used first-line treatment for ovulation induction. It’s been in use since the 1960s.
It’s used for women with normal hormone levels but no ovulation. This includes those with unexplained fertility, mild endometriosis, or luteal phase defects.
Here’s how it works. Clomiphene citrate is a selective estrogen receptor modulator (SERM). It blocks estrogen receptors in the brain. This tricks the body into thinking estrogen levels are low. In response, the brain releases more follicle-stimulating hormones (FSH) and luteinizing hormone (LH). These hormones stimulate the ovaries to grow follicles and release an egg.
Know more: How Many Days After Clomid® Do You Ovulate?
Here’s something important to know: even as estrogen levels rise later in the cycle, the brain doesn’t reduce hormone production. That’s because estrogen receptors stay blocked, allowing continued stimulation of egg development.
Clomid® contains two components that behave differently in the body. One is cleared quickly, while the other can remain for several weeks. Because of this longer-lasting component, Clomid® may continue to affect the uterine lining and cervical mucus even after you’ve finished taking it.
The dose is usually 50-100 mg per day for 5 days, starting early in the menstrual cycle (typically on the third day). Dosage shouldn’t exceed 150 mg or be used for more than 6 treatment cycles.
The live birth rate with clomiphene citrate is around 23.3% per treatment cycle.
Know more: 10 Tips for Getting Pregnant on Clomid®
Letrozole (Femara®)
Letrozole is an aromatase inhibitor, a newer class of medication introduced in 2001. It works differently from clomiphene.
Instead of blocking estrogen receptors, letrozole blocks the enzyme that converts androgens to estrogen. This lowers estrogen levels, which prompts the brain to release more follicle-stimulating hormone (FSH) and stimulate follicle growth.
Because letrozole clears from the body more quickly than clomiphene, it has fewer effects on the uterine lining and cervical mucus. That makes conception more likely once the egg is released.
This medication is especially useful for:
- Women with PCOS
- Women who don’t respond to clomiphene
- Older women trying to conceive
- Poor responders to standard fertility treatments
The typical start dose is 2.5 mg per day for 5 days, early in the menstrual cycle. The dose may increase to 7.5 mg if needed.
Another similar medication, anastrozole, has been studied at doses ranging from 1 to 15 mg per day for the same duration. Like letrozole, it’s used as an aromatase inhibitor for ovulation induction.
Letrozole tends to outperform clomiphene for women with PCOS. Studies show:
- The ovulation rate is higher with letrozole than with clomiphene — 61 – 80% vs. 48-68%.
- Live birth rates with letrozole are higher than with clomiphene.
Letrozole wasn’t originally developed for fertility treatment. But it’s now widely used and well-studied for ovulation induction.
Know more: Clomid® vs. Letrozole: A Complete Comparison
Tamoxifen
Tamoxifen is another oral option. It’s mainly used when clomiphene hasn’t worked.
Studies show that miscarriage rates are lower in women who conceive with tamoxifen or letrozole compared to clomiphene citrate.
Metformin
Metformin is an insulin-sensitizing drug.
Since many women with PCOS have insulin resistance, metformin was once thought to help with ovulation induction. However, current evidence shows its benefits are limited.
It’s mainly useful for women who don’t respond to clomiphene alone.
Know more: Metformin for PCOS: Fertility Benefits You Need to Know
Injectable medications
When oral medications don’t work, injectable hormones are the next step.
Gonadotropins directly stimulate the ovaries to grow follicles. (These include human menopausal gonadotropins (hMG) and FSH injections.)
Gonadotropin-based protocols produce the highest ovulation rates of all, reaching 90% or more in monitored treatment cycles.
However, they also carry a higher risk of ovarian hyperstimulation and multiple pregnancy. This is why close ultrasound monitoring is essential during every injectable cycle.
Surgical option: laparoscopic ovarian drilling
For patients with PCOS who don’t respond to medications, there is a surgical option called laparoscopic ovarian drilling (LOD).
This is a minimally invasive procedure. Small changes are made to the surface of the ovary to reduce androgen production and trigger normal ovulation. The exact mechanism isn’t fully understood, but long-term studies confirm it’s safe and effective.
Studies show LOD has success rates similar to gonadotropin therapy, making it a valid second-line option when medications haven’t worked.
Who May Not Be Suitable for Ovulation Induction?
Key Point: Ovulation induction may not be suitable for women with low ovarian reserve, severe infertility, or certain genetic conditions.
Ovulation induction won’t work for everyone. Some conditions make it unsuitable or unsafe.
It’s generally not recommended for women with:
Premature ovarian failure or poor ovarian reserve
Liver disease
Large ovarian cysts (greater than 5 cm)
Blocked or damaged fallopian tubes
Severe male factor infertility
Severe endometriosis (advanced stages)
Genetic conditions such as Turner syndrome
Pregnancy or breastfeeding (letrozole in particular may cause birth defects if taken during pregnancy)
Certain hormonal conditions where stimulating the ovaries won’t produce a response
If any of these apply, your doctor will discuss alternative paths, such as IVF or donor eggs.
What Is the Ovulation Induction Success Rate?
Key Point: Success rates depend on several different factors. But most women with ovulatory disorders respond well to treatment.
Success rates vary by age, cause of infertility, and treatment type. But the numbers are encouraging!
Here’s a quick comparison.
Medication | Ovulation Rate | Live Birth Rate |
Clomiphene citrate | 48-68% | 19.1% |
Letrozole | 27.5% | |
Gonadotropins | 90%+ | Varies by case |
A few things to keep in mind:
- Success rates are higher among young women and among women closer to a healthy body weight.
- Results tend to improve over multiple cycles, not just a single cycle.
- Combining ovulation induction with IUI can further boost the chances of conception.
- Women with PCOS tend to respond especially well to letrozole
What Are the Risks and Side Effects of Ovulation Induction?
Key Point: Ovulation induction is usually well-tolerated, but multiple pregnancy and ovarian hyperstimulation are real risks that careful monitoring helps prevent.
Ovulation induction is generally safe. But it does come with some risks worth knowing about.
Common side effects
Most women tolerate ovulation induction medications well. The most common side effects include:
- Hot flashes
- Headaches
- Fatigue
- Dizziness
- Mood swings
- Nausea
- Breast tenderness
These are usually mild and go away after the treatment cycle ends.
Medical risks
Some of the risks of ovulation induction include:
- Multiple pregnancy
- Ovarian hyperstimulation syndrome (OHSS)
- Ovarian enlargement and discomfort
- Miscarriage
How Much Does Ovulation Induction Cost?
Key Point: Oral medications are relatively affordable. Injectable cycles cost significantly more, especially when monitoring is factored in.
The cost of ovulation induction varies widely depending on the type of medication, monitoring required, and your clinic and country.
Here’s a general breakdown:
- Oral medications (clomiphene or letrozole): Relatively low cost. Letrozole and anastrozole tend to cost slightly more than clomiphene, but since they’re only taken for 5 days per cycle, the total drug cost stays manageable. This is especially true relative to the overall cost of a full treatment cycle, including stimulated IUI.
- Injectable medications (gonadotropins): Significantly higher cost. This is due to both the medication itself and the extra monitoring required.
- IUI or ART add-on: If timed intercourse is replaced with intrauterine insemination (IUI) or other assisted reproductive technology (ART), costs increase further
Most fertility centers will give you a full cost breakdown before you start. Exact pricing depends on your region and clinic protocol, so it’s always worth asking.
The Bottom Line
Induction of ovulation is a medical treatment that helps your ovaries do what they’re meant to do: grow and release a mature egg.
For women with PCOS, irregular ovulation, or unexplained infertility, ovulation induction is often the first and most effective step toward getting pregnant. With the right medication, close monitoring, and smart fertility tracking, most women respond well.
It’s important to keep in mind that personalized treatment matters. What works for one woman may not work for another. This is why working closely with your doctor to determine the right approach is so important.
You don’t have to do it alone. Track your hormones. Work with your doctor. And take it one cycle at a time.

FAQs
Ovulation induction itself is not painful.
Oral medications like clomiphene and letrozole are taken as pills and rarely cause physical discomfort.
Injectable medications, however, may cause mild soreness at the injection site. Some women feel bloating or pelvic pressure as follicles grow, but serious pain is uncommon.
If you feel severe abdominal pain during treatment, contact your doctor right away.
For women who aren’t ovulating, it’s one of the most effective first steps.
Ovulation induction is a well-studied, evidence-based treatment. It’s less invasive and less expensive than IVF.
For many women with PCOS or unexplained infertility, it can be enough to achieve a successful pregnancy.
The two most commonly used fertility drugs are clomiphene citrate (Clomid®) and letrozole (Femara®). Both are oral medications taken for 5 days early in the menstrual cycle.
Letrozole is often preferred for women with PCOS because it has higher ovulation and live birth rates.
Oral medications are taken as pills for 5 days, usually starting on the third day of the menstrual cycle.
Injectable gonadotropins are given as subcutaneous (under the skin) injections, usually starting early in the cycle.
Your doctor will guide you on exact timing, dose, and monitoring schedule.
It depends on the medication.
Clomiphene is typically used for up to 6 treatment cycles. If ovulation or pregnancy hasn’t happened by then, your doctor will usually switch to letrozole or injectable medications.
Letrozole cycles can also be repeated. How many depends on your individual response and your doctor’s guidance.
Your most fertile days are 6 days in total: 4 days before ovulation, the day of ovulation, and the day after ovulation.
If you’re going through ovulation induction, your doctor will use ultrasound and hormone tests to determine exactly when ovulation is happening.
Know more: Getting Pregnant: When Are You Most Fertile?
You can confirm ovulation through:
- Blood progesterone testing
- A sustained increase in urine PdG levels
- Ultrasound
Signs like egg-white cervical mucus, mild pelvic pain, increased libido, and a temperature rise after ovulation can also be helpful indicators.
For a convenient at-home option, PdG can be tracked with the Inito Fertility Monitor.
Know more: Fertility Myths vs Science: Ovulation, OPKs, and Timing
You can start with methods like the calendar method, tracking cervical mucus, or basal body temperature. However, these can be less reliable on their own.
For more accurate insight, tracking hormones like estrogen, LH, PdG, and FSH gives you a clearer picture of your cycle. This can be done easily at home with a device like the Inito Fertility Monitor.
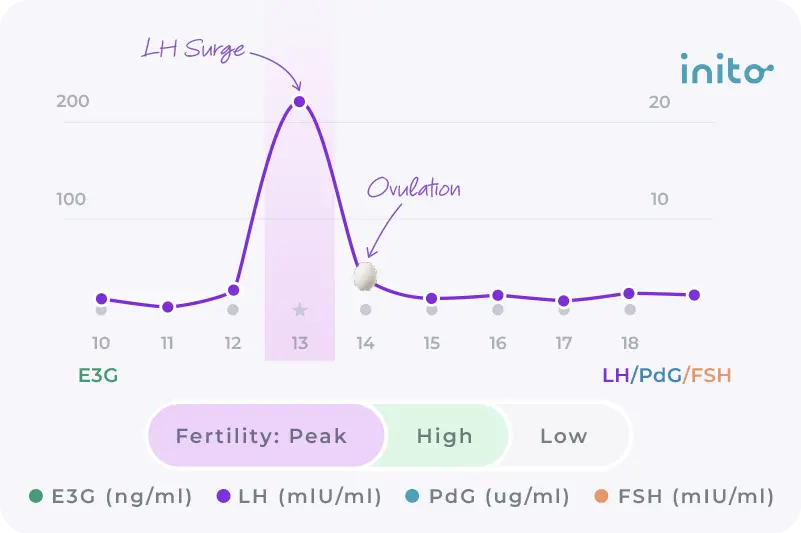
The only way to be sure you ovulated is to confirm a sustained rise in progesterone or its urine metabolite, PdG, after your LH surge.
A positive OPK only tells you ovulation is predicted. A steady and consistent rise in PdG rise tells you an egg was actually released.
Know more: PdG Test: What It Is + How to Tell If You Need One
Yes, it can increase the risk of twins or more. This is called multiple gestation.
It’s most common with injectable gonadotropins, which can stimulate multiple eggs developing and releasing at once.
Oral medications like letrozole carry a lower risk than clomiphene.
Careful monitoring helps reduce this risk.