Content table
Facts and fiction about sex have been passed down for centuries. You might have read online that certain sex positions will help you conceive.
Are there really any best sex positions to get pregnant that are scientifically backed, or just a myth?
Let’s get real: There’s a lot of misinformation online about sex positions and pregnancy. It’s hard to know who you can trust when you need accurate information about fertility.
Key Takeaways
- Conception involves ovulation, fertilization, and implantation.
- There’s no evidence that sex positions matter when you’re trying to conceive. As long as you’re having vaginal sex, you’re giving yourself a good chance of conceiving.
- Having penetrative sex around your fertile window is the best way to get pregnant quickly. Inito can help by tracking and confirming your ovulation.
- Other ways to get pregnant more quickly are to make good lifestyle changes.
- There are a lot of myths around having sex to conceive. Don’t trust everything you hear, and know that not every source on the internet is reliable.
Breaking Down Conception
To understand whether sex positions could improve your chances of conception, let’s get clear on what needs to happen for conception.
Ovulation
Ovulation happens when an egg is released from the ovary into the fallopian tube after maturing within a follicle. It occurs 12-14 days before your next period. You’re most likely to get pregnant in the days right around ovulation, so we like to call this your fertile window. Tracking your ovulation is one of the best ways to optimize your chances of getting pregnant.
If you don’t ovulate, you cannot conceive. Anovulation occurs when an egg is never released and can be caused by various factors.
Fertilization
Fertilization occurs when the sperm and the egg meet in the fallopian tube once you’ve ovulated and had sex.
You may have noticed that after you have sex, a lot of semen ends up on your sheets or your toilet paper. The sperm that remains may die inside the vagina if it doesn’t move quickly enough. Only the most agile sperm will ever see the fallopian tube, and only one needs to meet the egg.
Implantation
Pregnancy begins when the fertilized egg implants into the uterine lining.
The fertilized egg travels down the fallopian tube and into the uterus to plant itself on the endometrium. Here, the placenta begins to form and the fetus grows.
Learn More: Implantation: Everything You Need to Know
Key takeaways about conception
Making a baby may seem complicated but sex is the easiest part. Problems can arise at every point in the steps of conception. If you’re trying to conceive and having problems, it’s most likely not because of the sex positions you’re choosing.
On the other hand, there are ways to increase your chances of getting pregnant, and we’ll talk about those later. First, let’s talk about whether there’s a link between sex positions and conception.
Do Sex Positions Matter for Pregnancy?
There’s not a lot of evidence to support the idea that sex positions impact your ability to get pregnant.
Some experts say that positions for deep penetration will help your chances of conceiving. And this rationale does make sense: the further up the vaginal canal, the less distance sperm has to swim, right?
Yet there is no solid evidence to support this premise.
As long as you’re having vaginal sex, the position doesn’t seem to matter. This is because sperm are very motile. After they’re ejaculated into the vaginal canal, they surround and penetrate the cervix. Once inside, they don’t have far to travel to get to the fallopian tube.
The Best Sex Positions to Get Pregnant
The best sex positions for conception are the ones that work for you and your partner! Based on the best evidence we have, no one sex position will boost your chances of conception. So relax and enjoy your time in the bedroom!
But there are real ways to increase your chances of getting pregnant. Let’s talk about them.
How Can I Increase My Chances of Conceiving?
Even though sex positions don’t seem to matter, there are a lot of ways to enhance your fertility naturally.
Track Your Fertile Window
The best way to boost your odds of getting pregnant is to have sex during your fertile window. The days right before and after ovulation are your most fertile ones. Having sex in this window ensures that the sperm can meet the egg in the fallopian tube.
Tracking ovulation doesn’t just make sense, but it’s a proven way to get pregnant faster. In research, tracking ovulation helped participants get pregnant within just two cycles.
Read More: Getting pregnant: When are you most fertile?
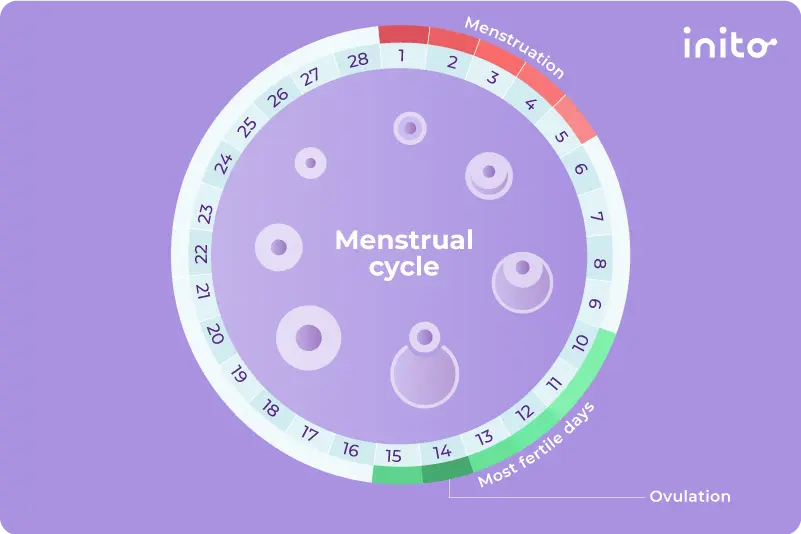
But how do you know whether or not you’re ovulating? It’s easier than you think. Here’s how:
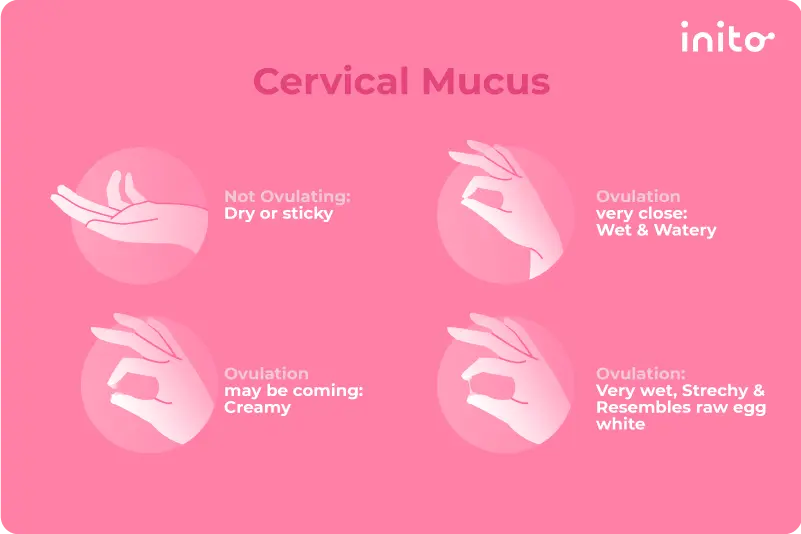
- Track your cervical mucus: The color and texture of your mucus can tell you a lot about where you are in your cycle. Learn how in our guide on cervical mucus.
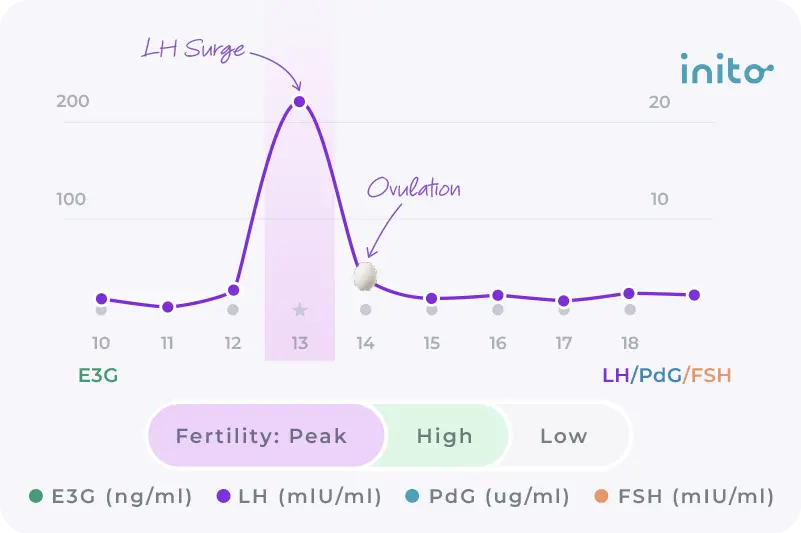
- Use advanced fertility tracking: Even when tracking your cervical mucus, it’s possible to think you’ve ovulated when you haven’t.
Inito’s advanced ovulation tracker confirms ovulation so you’re certain you have the best chance of conceiving.
Make positive lifestyle changes
We’re only recently starting to learn more about how our daily choices impact our fertility. Check out these factors that you can change to boost your chances of conception:
- Eat whole grains instead of refined carbs.
- Eat less meat and trans fats, as they have been shown to decrease fertility.
- Take a daily multivitamin, as these may help with ovulation.
- Maintaining a healthy BMI supports a normal fertility cycle.
- Exercise regularly to maintain an ideal body weight.
- Keep stress levels low.
- Quit smoking, which can inhibit ovulation.
- Get a regular pap smear.
Have sex more often
This may seem obvious, but getting intimate with your partner consistently and at the right time can help you get pregnant. In one study, participants who had sex more often increased their chances of getting pregnant within two years.
Common Myths and Facts About Sex Positions for Conception
You’ve probably heard or read about some of these common myths around sex positions and conception. Let’s bust some myths and make the facts clear.
Does having an orgasm increase your chances of getting pregnant?
There is little evidence to support that having an orgasm may help with sperm transport.
There are a few possible explanations for this. The hormone oxytocin rises during and after an orgasm, and may help sperm move from the vaginal canal through the cervix.
Yet many women don’t experience orgasms during vaginal sex. If you don’t orgasm during vaginal sex, don’t let this information stress you out.
There are other, more proven methods to improve fertility than having an orgasm. Women who orgasm from sex are no more likely to get pregnant than women who don’t.
Does the cervical direction matter for getting pregnant?
In order for sperm to travel to the fallopian tubes, it has to get through the cervix. Some people think that positions that widen the cervix may help more sperm get through. Others claim that the direction of your cervical opening can either help or harm your chances of conceiving.
There is no evidence that certain positions allow more sperm to reach the egg than others. There’s also no evidence that the direction of your cervical opening matters for conception.
Should I stay lying down after sex?
Some people say that lying down after sex allows the sperm to move through the cervix and into the fallopian tubes. There’s even advice out there to lie in bed with your legs above your head!
There is no evidence that these post-sex positions help with sperm motility. Viable sperm move quickly up the vaginal canal after ejaculation, so there’s no need for acrobatics to get them to the egg.
You may notice that some fluid falls out of your vagina after sex. When you pee, more of this fluid may fall out. Keep in mind that viable sperm are already in the cervix at this point. Losing excess semen and vaginal fluid is normal and doesn’t affect your fertility.
Read More: Peeing After Sex: Does peeing after sex push sperm out of the vagina?
Do certain sex positions “open up” the cervix?
Nope. The opening of the cervix (known as the cervical os) is a tight muscle. It doesn’t open during sex, but it does widen during ovulation and birth. A wider opening allows sperm to swim through the opening. It also lets a baby pass through during birth. This widening occurs because of hormones, not because of penetration.
Does deeper sex help with conception?
Conception does require vaginal penetration with ejaculation. In other words, you need to have sex to get pregnant. But there isn’t any evidence to suggest that deeper penetration helps with conception.
You may prefer deeper penetrative sex, or you may not. Neither is wrong. As long as your partner is ejaculating inside your vaginal canal, you have a good chance of getting pregnant.
Do lubricants help with conception?
Some people (and some lubricant companies) will tell you that lubricants help sperm move towards the egg. This information couldn’t be more false.
Sperm don’t have the motility to make it through thick lubricants. Many lubricants actually hurt or kill sperm before they even make it to the egg.
But if you prefer lubricants, you can still use them and get pregnant. Look for the “fertility friendly” label to be sure your lubricant isn’t toxic to sperm.
Do I need to have sex every day to get pregnant?
Nope. The most important time to have sex is during your fertile window. Having sex during the four days before ovulation, the day of ovulation, and one day after ovulation can help you get pregnant in that cycle. Having sex every single day is not only unnecessary, it’s often exhausting.

FAQs
The number of tests depends on the irregularity and length of your cycles. For someone with an average cycle length of 30 days, 12-15 tests may be required to track and confirm ovulation.
The number of tests depends on the irregularity and length of your cycles. For someone with an average cycle length of 30 days, 12-15 tests may be required to track and confirm ovulation.
The number of tests depends on the irregularity and length of your cycles. For someone with an average cycle length of 30 days, 12-15 tests may be required to track and confirm ovulation.
The number of tests depends on the irregularity and length of your cycles. For someone with an average cycle length of 30 days, 12-15 tests may be required to track and confirm ovulation.
There is no one most successful sex position for pregnancy. This is good news because it means you can opt for whatever positions are most enjoyable for you and your partner. To give yourself the best chance at pregnancy, the main thing to focus on is timing intercourse carefully within your fertile window.
Know more: When to Have Sex to Conceive
There’s not much you need to do during sex to increase chances of getting pregnant other than ensure ejaculation occurs. There are a lot of myths out there about orgasms, deep penetration, and laying down after sex leading to increased chances of pregnancy. But no research supports these claims. The best way to boost your chances of pregnancy is to make sure you have intercourse several times during your fertile window.
There’s no one particular position that has the highest chance of pregnancy. For better or worse, this is a myth that has no roots in scientific evidence. Focus instead on ensuring that you are tracking ovulation carefully and having sex on your fertile days.
No, missionary position is not bad for pregnancy. Different sex positions do not play a role in your ability to get pregnant as long as ejaculation occurs. So if you like missionary position, then go for it!
There is no sex position that increases the chance of pregnancy, so take this off of your list of things to worry about with trying to conceive! If you want to increase your chances of conception more reliably, make sure to track ovulation and have sex on your most fertile days.
The best position to get pregnant quickly is the position that is most pleasurable for you and your partner that will lead to ejaculation. No particular position is better than any other when it comes to getting pregnant—as long as ejaculation happens of course.
There is no sex position that has the highest pregnancy rate. As long as ejaculation occurs, your chances of pregnancy don’t vary based on the position. This means one less thing to worry about when it comes to trying to conceive. Yay!
The best way to do sex to get pregnant quickly is to track when you ovulate and to have sex several times within your fertile window. Inito can help you with tracking both ovulation and your fertile window (the 4 days before ovulation, the day of ovulation, and the day after ovulation).
Was this article helpful?
- Evbuomwan O, Chowdhury YS. Physiology, Cervical Dilation. [Updated 2021 May 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557582/
- Ikawa, M., Inoue, N., Benham, A. M., & Okabe, M. (2010). Fertilization: a sperm’s journey to and interaction with the oocyte. The Journal of clinical investigation, 120(4), 984–994. https://doi.org/10.1172/JCI41585
- Johnson, S., Stanford, J. B., Warren, G., Bond, S., Bench-Capon, S., & Zinaman, M. J. (2020). Increased Likelihood of Pregnancy Using an App-Connected Ovulation Test System: A Randomized Controlled Trial. Journal of women’s health (2002), 29(1), 84–90. https://doi.org/10.1089/jwh.2019.7850
- Kedzior, S., Bianco-Miotto, T., Breen, J., Diener, K. R., Donnelley, M., Dunning, K. R., Penno, M., Schjenken, J. E., Sharkey, D. J., Hodyl, N. A., Fullston, T., Gardiner, M., Brown, H. M., & Rumbold, A. R. (2019). It takes a community to conceive: an analysis of the scope, nature and accuracy of online sources of health information for couples trying to conceive. Reproductive biomedicine & society online, 9, 48–63. https://doi.org/10.1016/j.rbms.2019.08.004
- King, R., Dempsey, M., & Valentine, K. A. (2016). Measuring sperm backflow following female orgasm: a new method. Socioaffective neuroscience & psychology, 6, 31927. https://doi.org/10.3402/snp.v6.31927
- Kontula, O., & Miettinen, A. (2016). Determinants of female sexual orgasms. Socioaffective neuroscience & psychology, 6, 31624. https://doi.org/10.3402/snp.v6.31624
- Miller, D. J. (2018). Review: The epic journey of sperm through the female reproductive tract. Animal, 12. https://doi.org/10.1017/s1751731118000526
- Sharma, R., Biedenharn, K. R., Fedor, J. M., & Agarwal, A. (2013). Lifestyle factors and reproductive health: taking control of your fertility. Reproductive biology and endocrinology : RB&E, 11, 66. https://doi.org/10.1186/1477-7827-11-66
- Soumpasis, I., Grace, B., & Johnson, S. (2020). Real-life insights on menstrual cycles and ovulation using big data. Human reproduction open, 2020(2), hoaa011. https://doi.org/10.1093/hropen/hoaa011
- Steiner, A. Z., Long, D. L., Tanner, C., & Herring, A. H. (2012). Effect of vaginal lubricants on natural fertility. Obstetrics and gynecology, 120(1), 44–51. https://doi.org/10.1097/AOG.0b013e31825b87ae
- Thijssen, A., Meier, A., Panis, K., & Ombelet, W. (2014). ‘Fertility Awareness-Based Methods’ and subfertility: a systematic review. Facts, views & vision in ObGyn, 6(3), 113–123.