Content table
Around 7% of women experience an ovarian cyst at some point, so if you have questions about ovarian cysts and infertility, you’re not alone.
Some ovarian cysts may be associated with decreased fertility because they can affect a woman’s hormones or ovulation cycle.
As per the American Society for Reproductive Medicine, ovulation dysfunction accounts for one in four infertility cases.
So, which types of cysts are problematic, and how do cysts form in the first place? Here you will find answers to these questions and learn how to manage or identify the symptoms.
Key Takeaways
- Ovarian cysts may form in your body naturally as a part of normal reproduction.
- Most ovarian cysts are harmless.
- Some cysts can be associated with certain medical conditions that cause problems, such as hormone imbalances. Abnormal hormone levels can be related to infertility.
- In rare emergencies, cysts can rupture or cause damage to the ovary.
What are ovarian cysts?
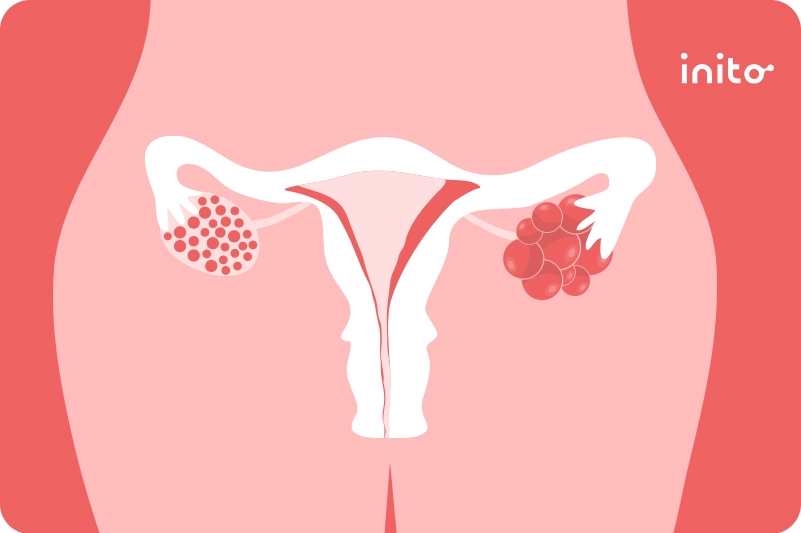
Ovarian cysts are fluid-filled sacs that can develop inside the ovaries. Cysts can vary in size, from as small as a pea to as large as a cantaloupe.
Also, they can occur alone or in clusters. Most ovarian cysts are benign (noncancerous). Yet, some can be malignant (cancerous) ovarian cysts.
Types of Ovarian Cysts
To understand this, you must first understand the female reproductive cycle. Typically, the follicles in a woman’s ovaries grow and release an egg cell about 12-14 days before the next cycle.
The egg comes from a small, fluid-filled sac inside the ovary called an ovarian follicle. The follicle fluid protects the egg as it grows and eventually, it breaks open to release the egg into the fallopian tube.
Cysts can form when the follicle doesn’t burst and the sac continues growing inside the ovary. They can also form after the egg is released if the sac doesn’t go away on its own. It keeps swelling and the fluid collects. This can lead to ovarian cysts.
Hormonal imbalances and certain conditions can also encourage cysts to form. Fertility drugs can also cause multiple follicles (cysts) to develop in the ovaries.
Types of ovarian cysts
Some ovarian cysts are more common than others. Here’s a look at the different types and what causes ovarian cysts.
Functional cysts
Cysts that form each month as and when the follicle grows are called functional ovarian cysts. These are common and are a regular part of the menstrual cycle. Usually, they are harmless and do not affect fertility.
There are two types of functional cysts: follicular and corpus luteum cysts.
Follicular cysts
These are the most common types of ovarian cysts. When the ovarian follicle fails to release its egg, it may continue to swell into a large follicular cyst. Most follicular ovarian cysts grow to be 2–5 cm in diameter or larger, then go away on their own. In rare cases, they can become larger and may require surgery.
Corpus luteum cysts
After ovulation, the empty sac forms what is called the corpus luteum. This corpus luteum makes hormones to prepare the body for pregnancy.
Usually, if the egg is not fertilized, it breaks down. But sometimes, it doesn’t dissolve. Instead, it begins filling with fluid and forms a corpus luteum cyst.
Over time, these cysts go away on their own, usually within a few months. However, they can grow to be large and cause pelvic pain and bleeding.
Non-functional cysts
Any other kind of cyst is considered abnormal. In some cases, they can be serious and may adversely affect your fertility.
Hemorrhagic cysts
Doctors don’t know why this happens, and most often, hemorrhagic cysts do not cause symptoms. In fact, women may not even be aware that they have them.
Hemorrhagic cysts typically resolve on their own.
Endometriomas
These are cysts that form in endometriosis, a condition in which uterine tissue called the endometrium starts growing outside the uterus. It is usually associated with low progesterone levels. These types of ovarian cysts may be linked with fertility issues.
- Ovarian cysts caused by polycystic ovary syndrome
Polycystic ovary syndrome (PCOS) is a medical condition in which small cysts develop on the ovaries. It can cause irregular periods and make it difficult to get pregnant. That’s because PCOS interferes with how your eggs are released from your ovaries. PCOS is associated with an excess of male hormones, like testosterone, called androgens.
| Type of cyst | Associated fertility changes | Associated hormonal changes |
| Functional cysts | ||
| Follicular cyst | No effect | No effect |
| Corpus luteum | No effect | Increased estrogen and progesterone |
| Non-functional cysts | ||
| Hemorrhagic | No effect | No effect |
| Endometriomas | Reduced fertility | Increased estrogen, decreased progesterone |
| PCOS | Reduced fertility | Increased testosterone and other androgens |
Can Ovarian Cysts Cause Infertility?
Some types of ovarian cysts are associated with hormonal imbalances that affect your ability to get pregnant. For instance, endometriomas can affect fertility. Also PCOS hampers your ability to get pregnant.
Moreover, the size, number, and location of the cysts can cause complications. In severe cases, ovarian cysts may rupture. Internal bleeding from a ruptured cyst could lead to scarring and ovarian damage. It may interfere with ovulation or implantation.
Ovarian cysts can also block the fallopian tubes, which makes it difficult for sperm to reach the egg. In some cases, cysts produce hormones that can interfere with ovulation.
How Is an Ovarian Cyst Diagnosed?
If you have ovarian cyst symptoms, your doctor may use the following tests to diagnose ovarian cysts:
- Pelvic exam: During a pelvic exam, your doctor may feel inside your lower abdomen for lumps or changes.
- Ultrasound (sonogram): If your exam is abnormal or you have symptoms that suggest something is wrong, your doctor may order an ultrasound (US) to look inside the abdomen. Two types of US that may be used for cysts are the abdominal US and the transvaginal US.
- Laparoscopy: Laparoscopy is a minimally invasive technique that uses small cuts or incisions to insert a small, lighted instrument into the pelvic cavity to view the ovaries and look for abnormalities.
How Can I Manage Ovarian Cysts?
If you are diagnosed with an ovarian cyst, visit your doctor regularly so they can monitor your cyst and provide treatment when necessary.
Remember that most cysts are harmless. Depending on your age, the size and type of cyst you have, and your symptoms, treatment may vary.
Watchful waiting
Most often, conservative management is the best way to treat ovarian cysts. If you have a small cyst with no symptoms, your doctor will likely recommend waiting a few months to see if the cyst resolves on its own. You may need several follow-up exams to check whether your cyst changes in size or appearance.
Medicine
Hormonal contraceptives, or birth control pills, prevent you from ovulating. In other words, they could stop you from getting more ovarian cysts. Also, if ovarian cysts are causing pain, you can take over-the-counter pain medicines for relief.
Surgery
If your cyst is not functional and is growing or causing pain, your provider may suggest removing it. In some cases, only the cyst needs to be removed (cystectomy), but in other cases, the ovary, along with the attached cyst, may also need to be removed (oophorectomy).
Studies show that surgery to remove a cyst is often more harmful than the cyst itself. A minimally invasive laparoscopic procedure is the best option if a surgical procedure is required.
Laparoscopy is performed using a thin, telescope-like device and instruments inserted through small incisions in the abdomen. Open surgery may be required if the cyst is too large to remove through the small incisions or if cancer is present.
When do ovarian cysts require medical intervention?
If you have the following symptoms after being diagnosed with an ovarian cyst, you might need a doctor’s evaluation:
- Pelvic pain that is dull, aching, or sharp in the lower abdomen, where the cyst is
- A feeling of fullness or heaviness in your lower abdomen/pelvic region
- Abdominal bloating or swelling
- Your doctor can perform an examination and advise you on the next steps
If left unchecked, some ovarian cysts can grow to the point where they pull on the ovary. This may lead to painful ovarian torsion (twisting) of the ovary, disrupting blood flow. Cysts can also rupture, causing severe pain and internal bleeding.
Seek immediate medical attention if you experience these symptoms:
- Sudden, severe abdominal or pelvic pain
- Fever or vomiting
- Signs of shock such as cold and clammy skin, dizziness, or rapid breathing
- These symptoms could indicate that the cyst has ruptured, or caused the ovary to twist (ovarian torsion).
FAQs
There are a variety of causes for ovarian cysts. These include:
- Abnormal growth of a follicle that doesn’t release an egg (follicular cysts)
- When a released egg fails to dissolve and instead fills with fluid (corpus luteum cysts)
- When a released egg fills with blood (hemorrhagic cysts)
- Conditions like endometriosis or polycystic ovary syndrome (PCOS)
In the majority of cases, ovarian cysts aren’t anything to be overly worried about. Often, they go away on their own, or they just remain without causing any issues. However, in rare cases, an ovarian cyst can be cancerous, infected, or rupture and damage the ovary or blood vessels.
In the case of harmless ovarian cysts, you’re not likely to have any noticeable warning signs. If the ovarian cyst ruptures or interferes with the blood supply to the ovary, you could notice the following symptoms:
- Pelvic pain or painful intercourse
- Increased urination
- Trouble emptying your bowels
- Periods that are irregular, heavier, or lighter than usual
- A bloated-looking or swollen belly
- The sensation of feeling full, even if you didn’t eat much
- Fertility challenges
The best treatment for an ovarian cyst depends on your symptoms as well as the size of the cyst. If you don’t have symptoms and your cyst is small, your doctor will likely just carefully monitor you and see if the cyst has changed after a few months. If a cyst is causing discomfort, you may be prescribed pain medication. You could even be prescribed hormonal contraception to prevent ovulation so that additional cysts don’t form. In the case of cysts that are larger, more disruptive, and painful, you may undergo a surgery. Surgery can remove just the cyst or both the cyst and the ovary.
In many cases, having an ovarian cyst won’t mean having to make any changes to your normal activity. This is especially true for smaller cysts or cysts aren’t causing any pain or discomfort. If you have a larger cyst or one that’s causing noticeable symptoms, then it may be best to avoid:
- Contact sports
- Vigorous exercise
- Sexual intercourse (if sex is causing pain and putting pressure on the cyst)
Yes, some ovarian cysts go away on their own without any sort of intervention like surgery. However, if an ovarian cyst continues to grow larger or it causes symptoms like pelvic pain or disruptions to going to the bathroom, you may require medication or surgery.
Size is one factor to consider in whether or not to remove an ovarian cyst, but the larger it is, the more it may be at risk of rupturing and causing additional complications. Most cysts are between 2-5cm, so any cysts on the higher end of that spectrum or larger, may be considered for surgery. Smaller cysts that are causing symptoms like pain or frequent urination may also need to be removed.
You can’t really do anything to dissolve an ovarian cyst naturally. It’s something that the cyst will do on its own. That said, using hormonal contraception can help with preventing new cysts from forming by keeping you from ovulating.
Was this article helpful?
- Can ovarian cysts cause infertility | ccrmivf.com
- Current diagnosis and management of ovarian cysts | pubmed.ncbi.nlm.nih.gov
- Endometriosis and Infertility | pubmed.ncbi.nlm.nih.gov
- FAQ Fast Facts about Infertility | ASRM.org
- Laparoscopy | MedlinePlus
- Management of Ruptured Cysts | hopkinsmedicine.org
- Mayo Clinic Q & A Hemorrhagic Cysts | mayoclinic.org
- Ovarian Cyst: Symptoms and Causes | pennmedicine.org
- Ovarian Cysts | medlineplus.gov
- Ovarian Cysts | ocra.org
- Ovarian Cysts and Infertility: A Connection? | mayoclinic.org
- Ovarian Cysts Medications | medscape.com
- Ovarian Cysts Overview | InformedHealth.org
- Ovarian Cysts StatPearls | ncbi.nlm.nih.gov
- Ovarian Torsion | StatPearls
- Pelvic Exam | mayoclinic.org
- Polycystic Ovarian Syndrome | clevelandclinic.org
- Polycystic Ovarian Syndrome and Infertility | pubmed.ncbi.nlm.nih.gov
- Prevalence, incidence, and natural history of simple ovarian cysts | pubmed.ncbi.nlm.nih.gov
- Relationship between ovarian cysts and infertility | pubmed.ncbi.nlm.nih.gov
- Ultrasound | MedlinePlus