Content table
Cramps can be challenging to navigate, especially when they seem to come out of nowhere. While cramps are a common part of your menstrual cycle and a sign that your period may be coming, that’s not the only thing they signal.
So why would you have bad cramps but no period?
Cramps can be caused by many other things happening in your pelvic area. These include implantation, pelvic inflammatory disease, endometriosis, uterine fibroids, inflammatory bowel disease, and more.
Your pelvis is home to your uterus, ovaries, fallopian tubes, bladder, bowels, and pelvic floor muscles. All of these organs work together to keep things running smoothly in your body. But sometimes, issues with any of these parts can cause pelvic pain and cramps.
If you’re experiencing what you think are severe menstrual cramps but no period, this article is for you. Read to learn more about what these cramps may mean and how you can relieve them.
Key Takeaways
- Cramps don’t always mean you’re menstruating. Cramps but no period can signal implantation, or conditions like endometriosis, PID, fibroids, and more.
- Pelvic pain can occur due to several factors. That’s because your pelvis is home to multiple organs, and issues with those can lead to cramps.
- If you’re experiencing severe cramps, fever, unusual discharge, or blood in your urine or stool, talk to a doctor.
- Over-the-counter pain relievers, heat therapy, and warm baths can help alleviate mild cramps.
Do Cramps Without a Period Mean Pregnancy?
Yes, the cramps you’re experiencing may be early pregnancy cramps.
Some reasons you may be feeling these period-like cramps during early pregnancy include implantation, changes in hormones, or an expanding uterus.
It can be challenging to distinguish between implantation cramps and period cramps. But here are some ways to help discern.
Period cramps tend to be dull or sudden. Implantation pain, on the other hand, may feel like mild pulling or tugging in your lower belly. That’s a sign that the fertilized egg is implanting in the lining of your uterus.
Learn more: What Do Implantation Cramps Feel Like?
Note: In the case of an ectopic pregnancy or miscarriage, you may also experience cramps. These are not your typical cramps, however. They are more severe, sudden, and stabbing pains, and happen on one side of your lower abdomen. These are both serious situations and require immediate medical attention.
What Are Other Causes for Bad Cramps, No Period?
Since there are so many organs in your pelvis, there are lots of reasons why you may have cramps but no period.
Here are some of the most common cramp offenders that occur with a phantom period:
Pelvic Inflammatory Disease (PID)
PID is an infection of your reproductive organs, often caused by sexually transmitted bacteria. These bacteria (including chlamydia, gonorrhea, and Mycoplasma) cause inflammation.
Pelvic inflammatory disease also causes lower abdominal pain, cramps, irregular discharge, and nausea. You may also experience fever, painful sex, and irregular vaginal bleeding.
How to diagnose: Testing for PID involves a physical examination, vaginal or cervical swabs, or blood tests.
If you think you may have PID, it’s important to see a doctor as soon as possible, as early treatment with antibiotics is key.
Endometriosis
Endometriosis is a struggle for 10-15% of child-bearing age women.
This inflammatory condition happens when tissue that’s similar to the inner lining of your uterus starts growing outside of the uterus.
This misplaced tissue acts like normal tissue, thickening and breaking down every month. Which means it can lead to severe cramps that interfere with your daily life. These cramps can be so intense that some women faint from them.
While most people associate endometriosis with period pain, this pain can happen outside of your period, too.
Endo is also often associated with pain while peeing, painful bowel movements, and pain following sex. Other symptoms include nausea and vomiting.
How to diagnose: Imaging, usually in the form of an ultrasound, is done to diagnose endometriosis.
Learn more: Your Guide to Getting Pregnant With Endometriosis
Irritable Bowel Syndrome (IBS)
This chronic digestive disorder causes abdominal or pelvic pain, bloating, and changes in bowel movements. Irritable bowel syndrome affects 10-15% of people in the U.S. and is twice as common in women as it is in men.
IBS feels like:
- Sharp pain
- Cramping
- Bloating
- Abdominal pain that’s like a burning sensation
- Distention
- Fullness
These symptoms are often triggered by eating specific foods and may come after a meal. However, those aren’t the only culprits. IBS can also be a result of emotional stress, constipation, or diarrhea.
How to diagnose: Symptoms are often used to diagnose IBS, as well as a blood test and stool test.
Uterine fibroids
These are non-cancerous growths developing from the muscular layer of the uterus. Small uterine fibroids may pass unnoticed and cause no problems. However, larger ones can push against other organs and cause pain and heavy menstrual bleeding.
How to diagnose: Imagery, such as an ultrasound, is used to diagnose uterine fibroids.
Ovarian cysts
These are fluid-filled sacs that form on one or both ovaries. They can lead to pelvic cramping that ranges from a dull aching sensation to a more intense pain. And that typically happens on one side of your pelvis.
Ovarian cysts can also leave you feeling bloated and a sense of pressure. The good news is that most of these cysts are harmless. But, there is the rare possibility that a cyst can burst. So if you have sudden and severe pain, seek medical attention.
How to diagnose: Testing for an ovarian cyst usually involves a pelvic exam and imaging.
Pelvic floor muscle dysfunction
Your pelvic floor muscles provides support to your uterus, bladder, and bowels. Trauma from childbirth, an accident, or even straining during heavy lifting, can affect these muscles and cause them to cramp. This leads to sudden lower abdominal pain.
How to diagnose: A physical pelvic or rectal exam is usually used to test for pelvic floor muscle dysfunction. Doctors may also use other tests such as electromyography (EMG) and an ultrasound or MRI.
Interstitial cystitis (IC)
This condition involves an inflamed or irritated bladder wall. The pain and discomfort tend to get worse as your bladder fills up.
How to diagnose: A variety of tests and exams are used to diagnose interstitial cystitis. These include a urinalysis, physical examination, cystoscopy, and additional tests.
How Do You Relieve Cramps?
- Over-the-counter pain medication. Drugs like ibuprofen or acetaminophen can help manage pain from cramps.
- Warm compress or hot water bottles. The heat from warm compresses or heat pads can help relax your muscles and ease cramps.
- Warm baths. Soaking in a warm water bath can be soothing and help reduce cramp pains.
- Hydration. Cramps can also be a result of dehydration. To avoid this, stay hydrated. Aim to drink approximately half your body weight in ounces of water per day.
- Relaxation techniques. Cramps can also be exacerbated by stress. Keep mild cramps at bay by practicing relaxation techniques like meditation, yoga, and slow, deep breathing.
- Tea. The herbs in specific teas can help reduce cramp pain. The best teas for cramps are ginger, chamomile, peppermint, and red raspberry leaf.
When Should I See a Doctor?
If you experience any of the following, don’t hesitate to contact your healthcare provider.
- Severe cramps that affect your daily activities
- Fever
- Foul-smelling vaginal discharge
- Blood in your urine or stool

FAQs
About 69% of women have up to 6-day variations in the menstrual cycle. This is totally normal! So your period could be just around the corner.
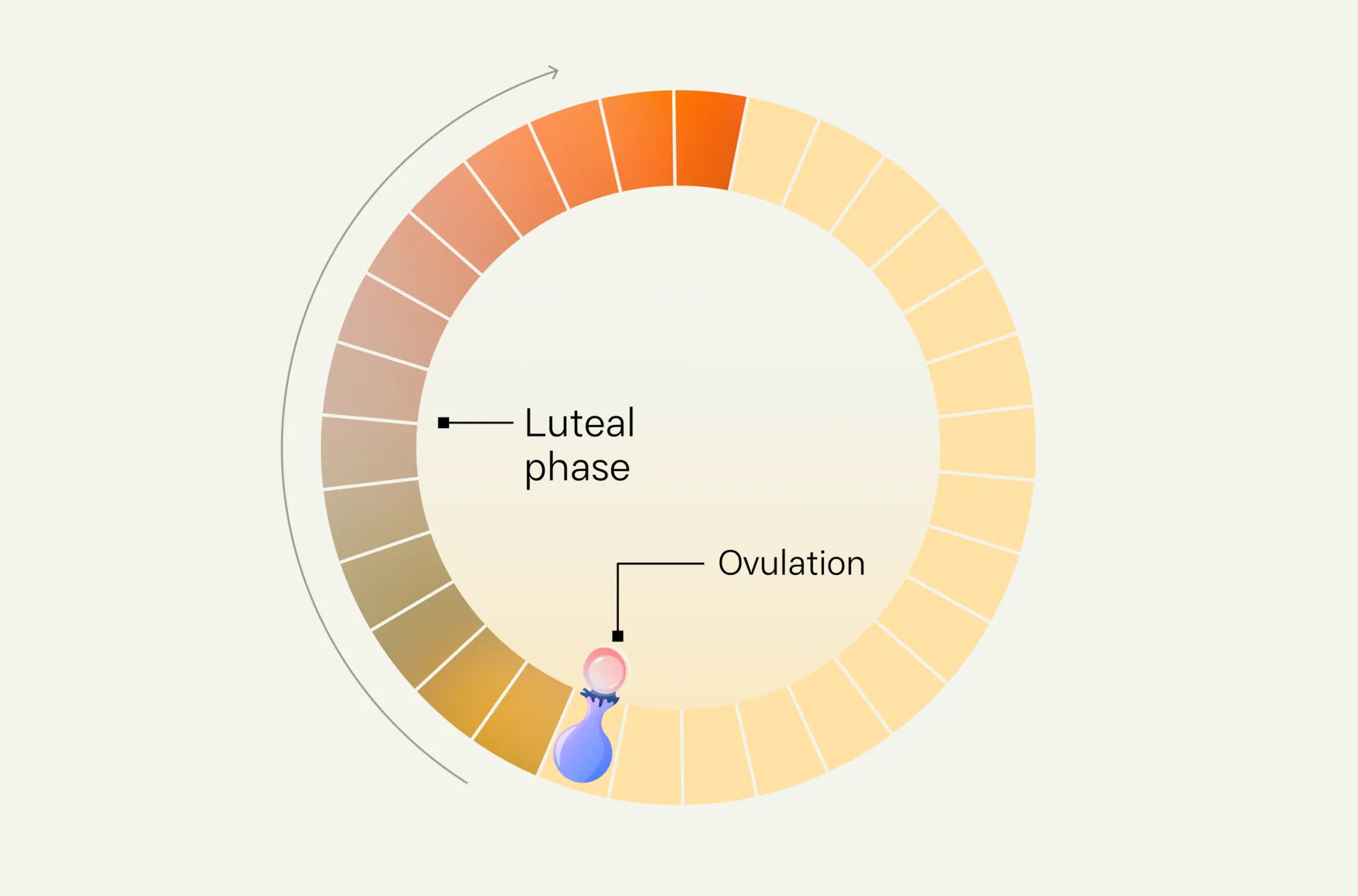
If that’s not the case, there are a few other reasons why you may be experiencing cramps but no period. You could be pregnant. Or you could be experiencing pain due to ovulation. You may also have a condition or issue for which cramps are a symptom. These include endometriosis, PCOS, IBS, cysts, uterine fibroids, PID, and more
This depends on how late your periods are. If you had sex during your fertile window and you’re late by more than a week, then yes, it’s better to take a pregnancy test.
Implantation cramps can last anywhere from a few hours to two days.
Certain conditions can cause cramping even after your period has ended. These include endometriosis, PID, IBS, ovarian cyst, or uterine fibroids. You may also be experiencing ovulation cramps which occurs in about 40% of women.
If your period is late, it’s possible that your cramps simply started earlier in this cycle. It’s not uncommon to have slightly fluctuating cycles from month to month. That said, cramping that happens in the absence of your period could potentially be from another cause. Some of these include endometriosis, uterine fibroids, inflammatory bowel disease, pelvic inflammatory disease, or even implantation.
If you’re having the same sensations that you normally have before your period but no period, there are a few possibilities. First, it’s possible that your period is simply running a few days behind. The symptoms you feel before your period starts are mainly due to your rising progesterone levels. So even if your period is late, you’d still experience that increase in progesterone and its associated symptoms.
Another possibility is that you could be in the early stages of pregnancy. Early pregnancy symptoms are very hard to distinguish from PMS symptoms because again, in both situations, the symptoms are mainly caused by high progesterone.
Outside of a late period or early pregnancy, it’s possible you have another underlying condition causing hormonal fluctuations and symptoms.
If you’re having severe period cramps along with fever, unusual discharge, or blood in your pee or stool, talk to your doctor ASAP. This could be a sign of an ectopic pregnancy or a miscarriage, and you should seek medical attention right away.
The cramping you feel during implantation and early pregnancy feels more like a short-lived mild pulling or tugging sensation that you feel on and off in your lower belly. Period cramps tend to be a little more intense and last longer.
There’s no true maximum delay for your period if you’re not pregnant because it depends on your unique cycle. If it’s been 6 weeks since day 1 of your last period, you likely had a missed period. And if you’re not pregnant, you’ll want to check in with your doctor.
When you experience high levels of stress while on your period, the length and amount you bleed may be irregular. You may also have more intense cramping than usual or experience other symptoms like headaches, fatigue, and trouble sleeping. These changes in your period are caused by fluctuating hormone levels that are triggered by increased stress levels.
If you’ve gone 6 weeks without having a period and you’re also not pregnant, you’ll want to talk to your doctor. Keep in mind that a little over two thirds of women experience variations in their cycle length by up to 6 days. So if your period is a week late, it’s usually no reason to worry. But if it’s been more than two weeks since your expected period and you haven’t tested positive on a pregnancy test, it’s pretty likely that you are not pregnant. And it could mean that you’ve had a missed period caused by anovulation or other hormonal issues.
In the two weeks after ovulation, it’s usually hard to tell for sure if you are pregnant or just late. This is because premenstrual symptoms and early pregnancy symptoms overlap since both are caused by rising progesterone levels. The only way to know for sure if you’re pregnant or late is to take a pregnancy test once the date of your expected period has passed.
Was this article helpful?
- Mittelschmerz | NIH
- About Pelvic Inflammatory Disease (PID) | CDC
- Endometriosis Is a Cause of Infertility. Does Reactive Oxygen Damage to Gametes and Embryos Play a Key Role in the Pathogenesis of Infertility Caused by Endometriosis? | Frontiers
- Irritable Bowel Syndrome (IBS) | American College of Gastroenterology
- Management of acute abdomen in pregnancy: current perspectives | Dovepress
- Abdominal pain during the menopause transition and early postmenopause: observations from the Seattle Midlife Women’s Health Study | Women’s Midlife Health Journal