Content table
hCG and miscarriage are closely related. If you’ve suffered a miscarriage, you may have heard your doctor talk about your hCG levels.
What do those levels indicate? Do they impact your ability to get pregnant again?
Here, we explain hCG and its relationship to miscarriage. This information may not ease the grief you’re feeling if you have had a miscarriage but it will help you understand what your body has been through. You’ll also be better prepared for your next pregnancy.
Let us first have a look at what hCG and miscarriage mean.
Key takeaways
- hCG levels usually follow a typical pattern during pregnancy. They rise rapidly for the first 10 weeks, then plateau and level off.
- Blood tests ordered by your doctor can detect hCG about one week after you become pregnant. Over-the-counter pregnancy tests are not accurate until around four weeks of pregnancy.
- When hCG levels show a slow rise or decline in early pregnancy, it means you may be having a miscarriage.
- Miscarriages are very common in the first trimester, affecting one-third of pregnancies.
- Doctors don’t usually track your hCG levels unless you have had a previous miscarriage or are having issues such as bleeding or cramping.
- After miscarriage, hCG levels usually return to normal in about four to six weeks.
- Most doctors recommend waiting a few months to become pregnant after a miscarriage.
What is HCG?
hCG, or Human Chorionic Gonadotropin, is one of several hormones in your body.
Small amounts of hCG are made in the pituitary gland, liver and colon. 20% of the hCG produced comes out through the urine.
Beta hCG is a hormone present in high amounts only during pregnancy. If your hCG levels are high and you are not pregnant, then you probably have ovarian or bladder cancer.
In men, high hCG levels are indicative of testicular cancer. During pregnancy, hCG takes on more significant role and helps the developing embryo get off to a good start. This is why hCG is often called the pregnancy hormone.
What is miscarriage?
A miscarriage is the loss of a developing fetus during the first 20 weeks of pregnancy. Most miscarriages occur in the first three months.
If you experience a miscarriage, your symptoms may include:
- Bleeding or spotting
- Back or abdominal pain or cramp
- Loss of mucus or clot-like tissue from your vagina
It’s important to call your doctor if you have any of these symptoms since a miscarriage can cause dangerous complications.
How does hCG work during pregnancy?
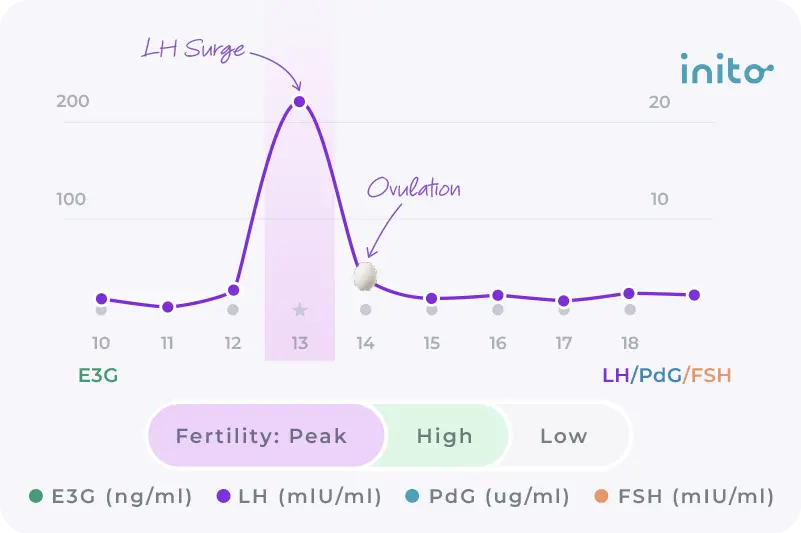
During your pregnancy journey, hCG peaks in the early stages, gradually drops down, and then levels off.
Shortly after the fertilized egg attaches to the wall of the uterus, the placenta starts making hCG. This, in turn, stimulates the production of another hormone called progesterone.
Progesterone helps support the development of the placenta. This tissue that sends blood and nutrients from your uterus to your growing baby.
As the placenta forms, it starts producing its own progesterone. Studies have found a link between progesterone levels and miscarriage as well.
After fertilization, hCG usually doubles every two to three days for the first four weeks. This slows slightly between weeks six and eight.
At about week 10, hCG levels peak then drop through the second trimester. For the rest of the pregnancy, they remain relatively constant.
A typical pattern of hCG through the first ten weeks of pregnancy is as follows:
|
Week # |
hCG Blood Levels (mIU/mL) |
|
3 |
5 – 72 |
|
4 |
10 – 708 |
|
5 |
217 – 8,245 |
|
6 |
152 – 32,177 |
|
7 |
4,059 – 153,767 |
|
8 |
31,366 – 149,094 |
|
9 |
59,109 – 135,901 |
|
10 |
44,186 – 170,409 |
How are hCG levels measured?
hCG can be measured in the blood and urine and its presence is understood to be an early indicator of pregnancy.
Your bloodstream absorbs hCG as it is produced. Some of it leaves your body through urine.
About one week after you become pregnant, a blood test by your doctor can detect hCG levels. Your hCG is usually < 5 mIU/mL if you are not pregnant. A level above 25 mIU/mL indicates pregnancy.
If your hCG is between 6 and 24 mIU/mL, your result is considered inconclusive. Your doctor will likely recheck your hCG in a few days to see if the level rises.
At-home pregnancy tests found in most drug stores measure hCG in your urine. However, you must note that they are not as sensitive as blood tests. While blood tests can be taken earlier, even before you have missed your period, a urine test to detect pregnancy is best taken after your missed period.
Do low hCG levels mean miscarriage?
Not necessarily. Baseline levels of hCG vary widely depending on many factors. One study found maternal smoking, your Body Mass Index (BMI), number of previous births, and gender of the fetus can all affect your hCG levels. Women who are pregnant with twins may also have higher levels of hCG.
What’s more important is how fast the levels are changing.
In early pregnancy, doctors look for your hCG levels to double every few days but they may not rise that fast. Research has found that 99% of pregnancies are still viable with an hCG rise of only 53% in two days.
Let’s break that down so it’s easier to understand.
When your hCG doubles, it increases by 100%. For an hCG level of 1,000 mIU/mL, a 100% increase would be 2,000 mIU/mL.
If it is increased by 53%, the hCG level would be 1,530 mIU/mL.
So, if your hCG level starts at 1,000 mIU/mL, the level should typically be 1,530 mIU/mL or higher two days later.
Your doctor will help you interpret your hCG test results and understand what they mean.
But don’t be concerned if your hCG isn’t rising as fast as you think it should. hCG levels can vary widely from person-to-person.
And does a slow rise in hCG mean miscarriage?
If the hCG levels are rising too slowly or decrease during the first trimester, it usually indicates an impending miscarriage. Sluggish or declining hCG levels can also be a sign of an ectopic pregnancy. This can be a dangerous condition, so your doctor will evaluate you carefully to find the cause.
However, hCG testing is not the only way to check your baby’s health. If your hCG levels seem off, your doctor may perform an ultrasound test to look for the baby’s heartbeat and assess the situation better.
Should I watch my hCG levels?
Doctors don’t usually track your hCG unless there’s a concern.
hCG is often measured to confirm a pregnancy, but it’s not checked regularly. If you have signs of a possible problem, such as bleeding or cramping, your doctor may check your hCG more often.
Routine hCG testing may also be helpful if you’ve previously had a miscarriage. Armed with knowledge about how hCG functions during pregnancy, testing will tell you whether your hCG levels are rising as they should. Having this information may give you peace of mind during this critical time of your pregnancy.
If routine testing shows your levels are not rising, your doctor can order other tests.
What you should know about hCG and miscarriage?
If you’ve suffered a miscarriage, you’re not alone. They are pretty common.
Most miscarriages happen in the first trimester (12 weeks). Doctors estimate that about three in 10 pregnancies end in miscarriage during this time. Many of these miscarriages happen to women who don’t even know they are pregnant yet.
Second-trimester miscarriages are less common. The risk of miscarriage during the second trimester is less than two percent.
What are the main causes of miscarriage?
Most miscarriages during the first trimester happen because of issues with the baby’s chromosomes that affect fetal development.
You have 23 pairs of chromosomes that carry all the genetic information you need to grow and live.
Chromosomes are passed on to your children through sperm and egg cells. Chromosomal defects can come from the sperm or egg. They can also occur if something goes wrong when the embryo is developing.
The other main causes of miscarriage during the first trimester of pregnancy include:
- Trauma from violent injuries or accidents
- Maternal health conditions such as uterine fibroids and endometriosis
In the second trimester, miscarriages can be caused by a variety of conditions, such as:
- Cervical insufficiency
- Infections
- Deformities of the fetus
- Preterm labor
What happens to hCG levels after miscarriage?
hCG levels decline after miscarriage, but it may take some time.
For most women, hCG declines to pre-pregnancy levels (< 5 mIU/mL) within four to six weeks after miscarriage.
How fast your levels return to normal may depend on when you miscarry.
For example, if the miscarriage occurs when hCG levels are at their peak, they may take longer to come down. On the other hand, if you miscarry when hCG is lower, your levels will return to normal quicker.
Can I become pregnant if my hCG levels are high after miscarriage?
Lingering hCG levels do not affect your ability to become pregnant again.
But they can interfere with future pregnancy tests. If you miscarry and then take a pregnancy test a few weeks later, you may still get a positive result.
This is because the pregnancy test picks up the hCG that’s still in your body.
Most doctors recommend waiting a few months after miscarriage to conceive again. Talk to your doctor about what’s right for you. Some factors to consider when thinking about trying for another baby include your:
Age: As you get older, your chances of getting pregnant decline.
Health: Your health and genetic factors may impact future pregnancies.
History of miscarriages and fertility issues: These may make getting pregnant more difficult.
Suffering a miscarriage can be a devastating experience. You may also need extra time to cope with your loss.
Was this article helpful?
Stat Pearls — Human Chorionic Gonadotropin—https://www.ncbi.nlm.nih.gov/books/NBK532950/
American Pregnancy Association — What is hCG? — https://americanpregnancy.org/getting-pregnant/hcg-levels/
Korevaar et al. — Reference ranges and determinants of total hCG levels during pregnancy: the Generation R Study — https://pubmed.ncbi.nlm.nih.gov/25963653/
Chung K, Allen R — The use of serial human chorionic gonadotropin levels to establish a viable or nonviable pregnancy — https://pubmed.ncbi.nlm.nih.gov/18825606/
Wilcox et al. — Incidence of early loss in pregnancy — https://pubmed.ncbi.nlm.nih.gov/3393170/
Mukherjee et al. — Risk of Miscarriage Among Black Women and White Women in a US Prospective Cohort Study — https://academic.oup.com/aje/article/177/11/1271/97504